COVID-19 Cancer services recovery plan 14 December 2020
Contents
- Background and purpose
- The current picture
- The Cancer Recovery Taskforce
- Plan on a page
- Success measures
- Planning for winter
- Key actions
- Appendix A: Supporting delivery of our Phase 3 aims
- Appendix B:How our approach aligns with the plans and priorities of the wider NHS
- Appendix C: Our key actions in Phase 1 – ensuring the continuity of urgent and essential services
- Appendix D: Our key actions in Phase 2 – supporting systems to start to return disrupted services
- Appendix E: Roles and responsibilities
- Appendix F: Governance
- Appendix G: Cancer Recovery Taskforce members
Classification: Official
Publications approval reference: C0821
NHS Cancer Programme
Cancer services recovery plan
14 December 2020
Background and purpose
The coronavirus pandemic has presented major challenges for all healthcare systems. One of the most significant impacts was a sharp reduction in the number of people coming forward and being referred urgently with suspected cancer and referred from screening programmes.
When coronavirus prevalence was at its highest at the start of the pandemic, this resulted in some people facing longer waits for diagnosis, some treatments being delivered in different ways or being interrupted or stopped on the grounds of clinical safety, and some follow-up care being disrupted.
Yet, thanks to the efforts of NHS staff and their partners, including many staff and volunteers in the cancer charities, the number of people receiving first or subsequent treatment was maintained at 86% of that in the same period in 2019 (March to September).
The response to the pandemic by NHS cancer services has focused on three phases (see Appendices B to D for further detail):
- Phase 1: ensure continuation of essential cancer treatment and screening for high risk individuals during the initial peak of the pandemic.
- Phase 2: restore disrupted services as far as possible to at least pre-pandemic levels.
- Phase 3 (to run until March 2021): full recovery of NHS cancer services in England, including ensuring that care for all patient groups continues to be safe, effective and holistic. This document sets out the national NHS plan to deliver this third phase. (See Appendices D and E for information on roles, responsibilities and governance for delivery of the plan.)
Equality and Health Inequalities Statement
Promoting equality and addressing health inequalities are at the heart of NHS England and NHS Improvement’s values. Throughout the development of the policies and processes cited in this document, we have:
- Given due regard to the need to eliminate discrimination, harassment and victimisation, to advance equality of opportunity, and to foster good relations between people who share a relevant protected characteristic (as cited under the Equality Act 2010) and those who do not share it; and,
- Given regard to the need to reduce inequalities between patients in access to, and outcomes from healthcare services and to ensure services are provided in an integrated way where this might reduce health inequalities.
The current picture
The principal reason for a reduction in the number of cancer patients commencing treatment was the fall in referrals.
Urgent referrals
The number of people seen following an urgent referral for cancer fell in April 2020, but by September had returned to 199,801 (102% of normal).
Waiting times
The number of people waiting more than 62 days for diagnostics and/or treatment following urgent referral has fallen by more than half but remains above the pre-pandemic level of about 11,800. This number peaked in May 2020 but by September had fallen to below 20,000, with continuing improvement. By tracking this number we can monitor the capacity of the system for diagnosis and treatment, and support regions and local systems if there is any suggestion they have insufficient capacity to meet demand.
Screening
The NHS breast and bowel screening services were locally paused in March 2020, but all services are now running across the country. The bowel screening programme is issuing screening invitations at rates over 100% of pre-COVID rates. There is still work to do to ensure the capacity is in place to manage patients that have experienced a delay during Covid-19.
Treatment
Most cancer treatment was maintained throughout the initial peak of the pandemic, although the need to protect patients from coronavirus infection and to manage the pressure on investigations, acute and critical care did disrupt pathways.
Over 291,000 people received their first or subsequent treatment for cancer during this time (March to September 2020), 86% of the number treated in the same period in 2019.
Over 150,000 people started their first treatment. This is around 30,000 fewer than in the same period last year, largely as a result of fewer referrals. Significant work has gone into encouraging people to come forward
The Cancer Recovery Taskforce
This plan has been developed with the Cancer Recovery Taskforce, which is chaired by Professor Peter Johnson, National Clinical Director for Cancer, and includes representatives from cancer charities, royal colleges, national teams and the NHS Cancer Programme’s Patient and Public Voices (PPV) Forum (see Appendix G for full membership).
The taskforce’s focus is the recovery of cancer services, and it reports to the National Cancer Board which oversees the delivery of the NHS Long Term Plan ambitions for cancer – to diagnose 75% cancers at stage 1 or 2, and for 55,000 more people to survive for five years or more, by 2028.
The taskforce’s roles are to:
- review progress against the aims of the recovery plan monthly, reporting to the National Cancer Board
- identify any requirements for the successful recovery of cancer services that are the responsibility of stakeholders outside the NHS Cancer Programme (eg public awareness, cancer screening, infection control measures)
- understand and represent the needs of patients and their families, and NHS staff, and engage with the wider cancer community on the national delivery of the recovery plan and its progress
- share practical suggestions about what the wider cancer community can do to support recovery.
The taskforce provides advice and guidance on national strategy for the recovery of cancer services. It also has an important role in representing the views of the cancer community in the wider national recovery strategy beyond cancer services, eg shielding.
The taskforce is monitoring progress against the aims of restoring demand, reducing waiting times and ensuring sufficient capacity for cancer diagnosis and treatment. Operational delivery resides with regional teams and STPs/ICSs, led and supported by the cancer alliances.
Plan on a page
| Aim 1. Restore demand to at least pre-pandemic levels | Aim 2. Reduce number of people waiting longer than they should | Aim 3. Ensure sufficient capacity to manage future demand |
|
|
|
We will achieve these key aims by:
| Supporting a ‘system-first’ model through alliances |
|
| Tackling inequalities |
|
| Ensuring public and staff confidence |
|
| Locking in innovations |
|
| Ensuring the right workforce is in place |
|
| Restarting LTP activity that supports recovery |
|
| Ensuring effective communications |
|
Success measures
Our success measures show what we want to achieve against each of our three aims.
| Aim | Success measure | Measurement |
| 1. Restore demand coming into the system to at least pre-pandemic levels | The number of patients to be seen in a first outpatient appointment following urgent GP referral will have returned to at least pre-pandemic levels | Monthly cancer waiting times data at national level (published)
Note: Progress on restoring screening programmes will continue to be measured and monitored through the national cancer screening programme boards |
| 2. Reduce the number of people waiting longer than they should for diagnostics and/or treatment at least to pre-pandemic levels on both screening and symptomatic pathways | The number of patients waiting more than 62 days after urgent referral will have returned to at least pre-pandemic levels | Monthly snapshot of the patient tracking list (PTL) at national level (published) |
| 3. Ensure sufficient capacity to manage future increased demand, including for follow-up care | The number of patients receiving first definitive treatment following a decision to treat will have returned to at least pre-pandemic levels | Monthly cancer waiting times data at national level (published) |
Where our data identifies issues with the progress being made, we will continue to work with regional teams to understand what they and their local partners are doing to respond, and will agree additional actions and support where necessary to ensure we see progress in all areas.
Ensuring we address ‘unmet need’
The drop in number of first treatments for cancer since the pandemic began indicates that some people who have cancer have not yet gone to their GP with symptoms or had a screening appointment. The NHS is acting to increase presentations to GPs and restore all cancer screening programmes.
As we monitor the number of people receiving first treatment – at national, regional and alliance level – we need to see the system ‘catch up’ with this unmet need, and by monitoring the waiting list over 62 days from urgent referral to see that capacity is sufficient to diagnose and treat all these people.
Planning for winter
COVID-19 infections in the community and hospitalisations are rising at different rates across the country, but as we approach winter we must stay focused on delivering the national plan for the recovery of cancer services by March 2021. We will continue to monitor progress across the country, with additional support offered to areas as they experience increased capacity challenges.
To help prepare for winter, we are asking cancer alliances to:
Maintain COVID-protected environments for cancer
- Ensure clear escalation plans are in place, with redeployment of staff involved in cancer screening, treatment and care considered only as a very last resort.
- Maintain or step back up cancer hubs for cancer surgery in line with existing advice.
- Use hub arrangements to protect capacity for endoscopy where possible.
- Maximise the use of independent sector capacity for cancer.
- Test non-symptomatic staff directly involved in the treatment and care of patients in cancer services on a weekly basis. Regularly test non-symptomatic patients attending chemotherapy and radiotherapy appointments (as advised by their clinical team), ensuring access to rapid testing at point of care for any patient who has not been tested or who has been unable to follow advice to isolate.
Continue to prioritise patient support, safety netting and use of clinical guidance
- Assign an individual patient navigator to each patient, as set out in the Adapt and Adopt blueprint for cancer.
- Continue to ensure appropriate local safety netting process is in place for patients where it has been necessary to postpone their treatment.
- Ensure paused clinical trials for cancer re-open as soon as possible and remain open.
- Where appropriate, make use of clinical guidance for symptomatic and screening services produced at the start of the year and during the pandemic, ensuring clinical decisions to stop or start treatment continue to be made according to the risk and benefit to the individual patient.
Maintain delivery of The Long Term Plan wherever possible
- Continue or resume the delivery of Targeted Lung Health Check projects.
- Implement at least one Rapid Diagnostic Centre pathway for a challenged two-week wait pathway, and one for patients with non-specific symptoms.
- Extend Personalised Stratified Follow Up programmes beyond breast, prostate and colorectal to support patients following their treatment and to increase clinical capacity by releasing outpatient slots.
Specific actions being taken at national level to support preparations for winter can be found under aim 3.
Key actions
Aim 1: Restore demand at least to pre-pandemic levels
To deliver this aim we will:
Run a major public awareness campaign:
- Ensure next phase of national ‘Help us help you’ campaign includes core cancer messaging, and that public-facing messaging on the importance of accessing NHS services continues throughout winter.
- Alliances, working with regional NHS England and Improvement public health commissioning teams where relevant, to lead and support delivery of local initiatives to increase referrals and screening uptake, eg patient ‘walk through’ videos.
- Provide consistent messaging to patients and the public on the safety of services, including screening services.
Ensure efficient routes into the NHS for people at risk of cancer:
- Through national communication and campaign efforts, as well as co-ordinated work locally, support the restoration and use of screening services. Ongoing restoration of the screening programmes will help to ensure the return to pre-pandemic standards as soon as possible.
- Encourage use of patient pathway navigators and other relevant actions through regional adapt and adopt plans.
- Support wider work on elective care to ensure that people with cancer not referred through an urgent cancer route receive timely diagnosis and treatment.
Improve referral management practice in primary and secondary care:
- Ensure focus on high quality referral activity, including safety netting, and identify and address unwarranted variation in referral access through key primary care contractual levers in the quality outcomes framework and network contract DES
- Disseminate, monitor and embed the use of guidance and tools that promote good practice in referral and safety netting activity, including to cancer alliance, PCN and primary care contacts, through a range of communication channels and as part of the commissioning framework for services.
- Through aligned national messaging, encourage effective communication and partnerships between primary and secondary care.
- Work in partnership with primary care at all levels to understand particular barriers to access as recovery is implemented, and identify opportunities for action.
Use this metric to track delivery:
- Number of patients seen in a first outpatient appointment following urgent referral from their GP.
Aim 2: Take immediate steps to reduce the number of people waiting over 62 days from urgent referral
To deliver this aim we will:
Audit and focus on longer waiters:
- Cancer alliances to lead local audit and prioritisation of longer waiters in line with clinical need (for patients on symptomatic and screening pathways) and ensure clinical harm reviews are undertaken.
- Ensure consistent application of cancer waiting times monitoring dataset guidance.
Implement urgent plans to increase/manage demand for endoscopy and imaging capacity:
- Enable implementation of innovations, such as using faecal immunochemical testing (FIT) as a triage tool, and telephone and video calls for specialist bowel screening practitioners.
- Provide £6m funding to cancer alliances to develop pilot Colon Capsule Endoscopy clinics. The clinics will use a small camera, which is swallowed by the patient, to film inside the body and identify any signs of cancer.
- Support delivery of high impact actions within endoscopy and imaging adapt and adopt blueprints.
- Cancer alliances to lead implementation of specific actions to help restore endoscopy capacity, including substituting CT colonography for colonoscopy where local circumstances permit, aligning infection prevention protocols locally and fully implementing polyp surveillance guidance.
Implement best practice and modified pathways to account for impact of COVID-19 and ensure patients are seen as quickly and as safely as possible:
- Cancer alliances to lead implementation of diagnostic pathway modifications and the RDC principles, including the use of ‘hot reporting’.
- Support full implementation of timed diagnostic pathways for lung, prostate, colorectal and oesophago-gastric cancers, and establish new timed pathways for head and neck and ovarian cancer.
- Prioritise treatment changes that deliver greater patient benefits, such as changes to the delivery of chemotherapy, and ensure improvements are ‘locked in’ for the future where appropriate.
- Continue to monitor the management of patients requiring more than one episode of treatment, to ensure those with recurrent/secondary cancer receive timely and appropriate care and treatment.
Use this metric to track delivery:
- Number of patients waiting over 62 days after urgent referral.
Note: The data source currently covers only urgent referrals, but we are looking to extend it to screening pathways.
Aim 3: Ensuring sufficient capacity to meet demand
To deliver this aim we will:
Maximise use of available capacity (on both symptomatic and screening pathways) through system-wide working:
- Cancer alliances to lead expansion of capacity of COVID-19 protected surgical hub arrangements and, where appropriate, local extension of whole-system models to other treatments (including palliative and end-of-life care) and diagnostics (this may be through the early development of community diagnostic hubs).
- Encourage delivery of relevant adapt and adopt cancer blueprint actions, eg use of alliance-wide PTLs where appropriate locally.
- Support wider approaches aimed at maximising available capacity, eg development of diagnostic networks.
Optimise use of available independent sector capacity:
- Monitor the use of diagnostic and treatment capacity within the independent sector contract, and support regions, alliances and providers to take advantage of independent sector capacity through national framework contracts from November 2020 onwards.
Enable restoration of other services:
- Cancer alliances to lead the resumption of any support, follow-up or other relevant services for those already diagnosed with cancer, that have been impacted by the pandemic.
Take action to protect service recovery in preparation for winter:
- Keep national clinical guidance under review. Issue advice to regions for specialised surgery, chemotherapy and radiotherapy.
- Work with cancer alliances to ensure readiness of cancer surgical hub arrangements across the country and the protection of diagnostic and treatment teams from redeployment.
- Work with NHS planning teams to optimise use of available independent sector capacity, particularly to support cancer surgery.
- Work with the taskforce to ensure appropriate COVID-19 testing for patients and staff. Monitor shielding advice and build this into public messaging.
Use this metric to track delivery:
- Number of patients receiving first definitive treatment following a decision to treat for all cancers.
Looking to 2021/22 and beyond
We remain committed to delivering the Long Term Plan ambitions for cancer:
- by 2028, 55,000 more people will survive cancer for five years or more each year; and
- by 2028, 75% of people will be diagnosed at an early stage (stage one or two).
As indicated in this plan, we are working to ensure that activity that will help us to meet these ambitions can continue during the pandemic, particularly through our major programmes of work, such as Rapid Diagnostic Centres and Targeted Lung Health Checks. In addition, we will want to capitalise on the innovations and new ways of working that have been developed as a result of the pandemic. As the recovery phase is completed, there will also be a renewed focus on securing sustainable delivery against the cancer waiting time standards.
We will continue to work with cancer alliances to support them to deliver change locally, for example through dedicated funding, provision of data and analysis, and best practice and tools. In addition, we will:
- work with relevant colleagues to ensure the additional £325m capital funding announced in the Spending Review for diagnostics in 2021/22, as well as the funding for elective care and workforce, supports delivery of the Long Term Plan ambitions for cancer; and
- continue to identify and roll out innovative approaches that will improve outcomes, including piloting a blood test, developed by GRAIL, that may detect early stage cancers.
Appendix A: Supporting delivery of our Phase 3 aims
Supporting a ‘system-first’ model
- Cancer alliances, with their local ICS/STP, and NHS England and Improvement reginal public health commission teams, will develop integrated local recovery plans, including screening, diagnostics and workforce. Nationally, we will share resources and best practice to support this.
- Cancer alliances will embed system-wide approaches to manage demand and capacity, including clinical triage, use of the independent sector and centralised booking and management systems.
- Nationally, we will provide weekly and monthly data packs with information on managing referral, diagnostics, treatment and longer waiter numbers to inform local planning and delivery.
- Nationally, we will run a monthly recovery check-in process to monitor and identify priority actions for regions and alliances.
Tackling inequalities
- Nationally, we will develop specific analysis and monitor our key recovery metrics by deprivation, age, sex and ethnicity, reviewing pre- and post-COVID-19 access levels to identify areas for urgent action. Nationally, we will continue to ask patients for their views through the NHS Cancer Programme PPV Forum, the Cancer Improvement Collaborative, cancer charity partners and non-cancer community organisations, and use this feedback to inform priority actions. We will ensure that patient feedback mechanisms are in place for decision-making at all levels.
- We will share the data and patient intelligence with alliances to inform local actions, and use them nationally to target our public awareness activity.
Ensuring public and staff confidence
- National teams and cancer alliances will promote the implementation of national guidance on reducing transmission of coronavirus in healthcare settings.
- Cancer alliances will monitor availability of testing, PPE and incidents of clinical harm. They will escalate issues and take appropriate local action.
- National teams and cancer alliances will use all communications channels to set out the steps the NHS is taking to maintain COVID-19 protected environments. Through their networks and channels, the Cancer Recovery Taskforce will help to amplify these messages as appropriate.
Prioritising innovations that support recovery
- National teams and cancer alliances will support the roll out of innovations accelerated as a result of the pandemic, such as stereotactic ablative radiotherapy (SABR), ‘COVID-friendly’ treatments and chemotherapy delivered in different settings.
- Nationally, we will enable robust evaluation of innovations and prioritise support from the 2020/21 Innovation Fund to roll out selected diagnostic interventions (with an early focus on endoscopy), and support delivery of best practice (eg in clinical decision-making, rule in/out tests).
- Cancer alliances will lead the local implementation of innovative solutions, supported by £4m funding.
- Nationally, we will work with the National Institute for Health Research to support the recovery of cancer clinical trials (including for children and young people) by summer 2021.
Ensuring the right workforce is in place
- Cancer alliances will support the deployment of cancer staff returning to the NHS through the bringing back staff scheme, and will pilot new NHS volunteer roles to support cancer patients.
- National teams and cancer alliances will encourage take up of Health Education England’s 2020/21 training grants for clinical nurse specialists and chemo-nurses and extra training places for other specialties highlighted in the People Plan, including developing an advanced clinical practice qualification in oncology.
- Cancer alliances will identify individuals nearing the symptomatic colonoscopy accreditation thresholds and support them to gain JAG accreditation.
- Cancer alliances will support flexible working innovations, such as workforce passports, remote reporting, seven-day working, additional lists for qualified staff and parallel running of old and new machines, as well as approaches to support NHS staff health and wellbeing.
- Cancer alliances will take action to retain and re-purpose the BowelScope workforce while the service remains suspended, and expand training opportunities for trainee lower GI endoscopists in the next 12 months.
- Cancer alliance will support clinical nurse specialists to work at the top of their licence by deploying an effective skill mix model, including cancer support worker and volunteer roles.Nationally, we will input to the spending review and prioritisation of funding.
Restarting Long Term Plan activity that supports recovery
- Cancer alliances will continue to develop and roll out RDCs in line with the RDC specification;
- Nationally, we will work with sites to enable the early resumption of the TLHC Programme, and ensure projects have access to sufficient CT capacity to be able to deliver the programme.
- Cancer alliances will build on their work on personalised stratified follow-up pathways across a range of cancers to support patients following treatment, and increase clinical capacity for new patients requiring treatment by releasing outpatient slots. Pathways are to include the use of remote surveillance and access back to their cancer team when patients need it. Personalised care, including access to patient education, is to be embedded alongside better support for self-management, to ensure individual and holistic patient needs are met.
Ensuring effective communication across the cancer community
- Nationally, we will run monthly webinars with cancer charities to brief them on progress and get their feedback on patient experience, and publish a regular stakeholder bulletin. We will also engage regularly with the NHS Cancer Programme’s PPV Forum.
- We will host monthly calls with cancer clinicians and cancer alliance clinical chairs, and continue to communicate regularly with cancer alliance managing directors.
Appendix B: How our approach aligns with the plans and priorities of the wider NHS
| Phase 1 | Phase 2 | Phase 3 | |
| National response |
|
|
COVID-19 incident response reduced to level 3, incident response services maintained |
| Wider NHS priorities |
|
|
|
| National cancer team key priorities |
|
|
|
| Planning |
|
|
|
Appendix C: Our key actions in Phase 1 – ensuring the continuity of urgent and essential services
Providing clear clinical and operational guidance
- Guidance issued March 23 on prioritisation of patients and organisation of services during the disruption.
- Letter sent to the NHS on the continuation of urgent and essential cancer treatment.
- Other guidance on management of urgent referrals and safety netting, screening, endoscopy, proton beam therapy and primary care.
Supporting the development of hubs for cancer surgery
- Worked with cancer alliances, regional teams and specialised commissioning to support and enable continuation of essential cancer services.
- Following guidance, surgical ‘hubs’ were developed in all 21 cancer alliance areas to provide surgical services in protected environments for cancer patients.
- Further work is underway to build on this model to deliver diagnostic services in protected environments.
Ensuring clear communications and engagement
- Worked as part of the national ‘Help us help you’ campaign to deliver key messages – in particular, that anyone with worrying symptoms should go to their GP. Urgent referrals have been rising steadily since the campaign began.
- Maintained regular channels of communication with key stakeholders, including updating FAQs for charities to use on their patient support lines.
Appendix D: Our key actions in Phase 2 – supporting systems to start to return disrupted services
Continuing clear communications and engagement
- Continued to promote cancer-specific messages as part of the ‘Help us help you’ campaign.
- Developed patient-facing messages on approaches being taken to reduce the risk of transmission in healthcare settings.
Providing clinical guidance and support
- Developed and shared a guide for the management of diagnostic services during the pandemic – including applying RDC principles and adapted diagnostic pathways.
- Developed and shared a guide for prioritisation and triage of patients with lower GI symptoms.
- Supported development of guidance on testing for asymptomatic staff and patients in non-surgical oncology in the UK.
Supporting new ways of delivering care and treatment
- Accelerated the implementation of the use of SABR, an innovative and life-saving type of radiotherapy, for use by the end of the financial year.
- Supported cancer alliances to use innovative approaches locally, such as FIT testing to triage lower GI referrals.
- Issued an amended service protocol for the delivery of TLHCs.
Developing analytical tools
- Developed and shared a national model to help alliances understand the potential scale of the demand for services in different scenarios.
Appendix E: Roles and responsibilities
| STPs/ICSs and cancer alliances |
|
| Regional teams |
|
| National team |
|
| Wider stakeholder community |
|
Appendix F: Governance
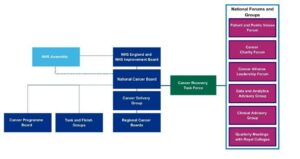
Appendix G: Cancer Recovery Taskforce members
-
- Blood Cancer Alliance
- Bowel Cancer UK
- Breast Cancer Now
- Cancer 52
- Cancer Research UK
- Children and Young People’s Cancer Charities Coalition
- Health Education England
- Less Survivable Cancers Taskforce
- Macmillan Cancer Support
- NHS Cancer Programme Patient and Public Voice Forum
- NHS England and NHS Improvement Public Health Commissioning and Operations
- Public Health England
- CMO
- Royal College of General Practitioners
- Royal College of Nursing
- Royal College of Pathologists
- Royal College of Physicians
- Royal College of Radiologists
- Royal College of Surgeons of England
