SARC requests for forensic medical examinations during COVID-19 pandemic
Contents
- SARC requests for forensic medical examinations (FMEs) during Covid-19 pandemic
- Videoconferencing
- Box 1. Forensic self-taken samples
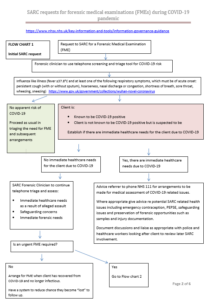
- Box 2. Telephone consultation Forensic Medical Examinations
SARC requests for forensic medical examinations (FMEs) during Covid-19 pandemic
The COVID-19 pandemic has created a situation that is highly dynamic. As such the advice given may change. We will be guided by Public Health England (PHE) and local protocols.
- Please be mindful of frequent COVID-19 updates.
- This guidance covers requests for forensic medical examinations.
- The processes below are new. There are likely to be issues that arise that have not been covered in this guidance. We will update based on events and feedback.
- These new processes effect other stakeholders such as police and for some SARCs other hospital departments, therefore local discussion and effective teamwork is essential.
- SARCs may want to work with local GUM departments to develop protocols for provision of more than 5 days’ worth of HIV PEP when it is required.
- Please have a low threshold for discussing issues with a senior member of the SARC team.
- A COVID-19 Telephone Screening and Triage tool should be used for any request for an FME.
- Use Flowcharts 1 and 2 below to assist with decision making around the management of cases.
- In cases where the client is being seen in SARC, where possible, whilst maintaining safe and caring practice, limit face to face contact, as some may be infectious whilst symptomless.
- Consider taking histories over the phone where possible.
- Limit those accompanying a client attending SARC to minimum.
- Ask all those attending SARC to wash their hands with soap and water on arrival.
- Minimise movement of attendees and limit them to rooms that can be deep cleaned.
- Keep as far as possible from others, including other SARC staff, professionals, clients and their family or friends.
- Ensure that your written records reflect the processes that you have undertaken.
- Please feedback anything that you think the team can learn from.
NHSX has produced guidance for health workers with regards to using technology to communicate with patients during this COVID-19 crisis. On videoconferencing it states, “We encourage the use of videoconferencing to carry out consultations with patients and service users. This could help to reduce the spread of COVID 19. It is fine to use video conferencing tools such as Skype, WhatsApp, Facetime as well as commercial products designed specifically for this purpose.
The consent of the patient or service user is implied by them accepting the invite and entering the consultation. But you should safeguard personal/confidential patient information in the same way you would with any other consultation.”
[FOLLOWING LINK NOT FOUND]
https://www.nhsx.nhs.uk/key-information-and-tools/information-governance-guidance

Box 1. Forensic self-taken samples
Ideally for SARC clients, any forensic samples would be either the routine EEK taken by police or those taken by a Forensic Clinician.
Self-taken samples by clients are not advocated other than in extreme circumstances.
There is a significant impact on the level of interpretation that a forensic scientist can provide regarding a self-taken sample.
Where a decision has been made that a face to face forensic medical examination is not possible and, having discussed the options with the police and client, the Forensic Clinician should decide if self-taken swabs are an option, bearing in mind the age of the client, menstrual status etc. If it has been decided that self-taken swabs are necessary then:
- Where possible, collect underwear and sanitary wear (these are more important than self-taken ano-genital samples).
- There is no need to take both internal and external samples from the vagina (and anus).
- The client need take only one sample from each area required (e.g. one low vaginal swab and one anal/rectal swab).
- Where skin swabs are required to be self-taken, consider any clothing worn over the area of interest at the time of the alleged incident or soon after, as this is likely to provide more robust evidence than self-taken swabs.
- Ensure the FME notes fully reflect the discussions and decisions.
- Ensure any paperwork associated with the forensic samples makes it clear which are self-taken.
- Ensure risk of contamination (in this case COVID-19) is clearly marked on samples and associated paperwork.
Box 2. Telephone consultation Forensic Medical Examinations
- This is clearly a very different process from normal.
- Note Page 1 of this document sets out that videoconferencing, e.g. use of Skype etc. may be considered.
- Remember others involved are likely to be stressed. Be kind to each other. Allocate more time than usual to ensure time pressures are less likely to be an issue.
- Ensure that you have correct phone numbers for police / client involved.
- Collect also the email addresses for police and where available the client (test email first) as useful e.g. for those whose hearing is impaired.
- Consider other communication difficulties.
- Make sure documentation accurately reflects the processes and conversations.
- Continue to use usual FME paperwork and processes as much as possible.
- When taking a history on the phone – ask and record who is in the room with the person you are talking to. Where possible have the client on their own where they can talk privately to SARC staff.
- Crisis worker to speak to client, outlining that the Forensic Clinician will get a history of events from police before speaking to the client. Crisis worker to go through usual paperwork including LDSQ and screen for DV as usual (mindful of who might be able to hear answers).
- Meanwhile the Forensic Clinician to take a history from the police officer.
- Forensic Clinician to discuss consent with client. As consent will not be written, the crisis worker should witness this process.
- Undertake a risk assessment regarding emergency contraception (and consider if needs double dose of Levonelle), HIV PEPSE, Hep B, suicide risk, imminent self-harm, safeguarding etc. the same as usual.
- Discuss the need for arrange for a third party (COVID-19 free) to attend SARC to collect EC or HIV PEP as necessary.
- If giving HIV PEP consider (in discussion with local GUM) providing more than 5 day pack.
- Complete prescriptions same as usual.
- Record batch numbers and expiry dates as usual practice.
- Give written information of STI GUM clinics and particularly for HIV PEPSE cases advise that the client will need to phone the clinics in good time as they too may be doing telephone consultations only.
- Discuss with the police what the forensic strategy will be (be mindful of Box 1).
- If self-taken swabs are required:
- Wear usual SARC PPE so as not to contaminate samples whilst preparing them.
- Fill out necessary paperwork, FFLM FME form or other local form, making it clear samples are SELF TAKEN and you have not seen the client due to COVID-19 risk.
- Record on FME forms the venue that self-taken swabs will take place at.
- Label samples and bags with:
- Date and your name/reference number.
- Client name and DOB.
- SARC number and nature of sample.
- SELF TAKEN COVID-19 risk.
- Place all required samples in their matching unsealed sample bags and place these in large evidence bag. Include water vial in case required and the pack of paper.
- Ideally underwear and sanitary wear will also be collected so add bags for that too.
- Place in a large evidence bag and seal.
- In a separate sample bag include an adequate number of gloves and a forensically clean pen.
- Place all of the above in a large brown evidence bag together with the exhibit forms.
- Arrange for the police to pick up the unused Forensic Samples and associated paperwork (keeping a copy of the latter in the forensic notes).
- Additionally give the attending police officer
- The relevant Patient Information Leaflet on Self-taken Samples
- The usual post FME SARC information leaflets.
- Where appropriate a SARC washbag.
- Any medication that has been determined as necessary.
- Your chain of evidence in the contemporaneous records should reflect what you have done.
- Discuss with the police if SOCO need to attend to document images.
- Be available to talk to the client as required when they are taking any self-taken samples.
- The client should:
- wear gloves when taking the samples
- place samples into the correct sample bags
- place the individual bags into one large evidence bag which should be sealed.
- The police officer handling samples should be double gloved and place the large sealed evidence bag into a paper evidence bag. They should then, without touching anything else, remove the outer gloves, place inside the paper evidence bag before sealing with bio-hazard tape, labelling as appropriate:
- Client details
- Continuity details
- COVID-19 risk.
- The police officer should carefully wash their hands with soap and water or alcohol gel if soap not available, after handling the sample bags.
- Coronavirus is not destroyed by freezing, therefore the risk of infection remains with frozen samples. Therefore samples should be stored in a manner that minimises future risk. Any handling of the bags should be done using double gloves and followed by careful cleaning.
- At the end of this episode, the Forensic Clinician should talk through with the police officer at the scene what forensic samples have been collected and make a record in the notes.
- The Forensic Clinician should discuss with the client:
- Any medication that you have sent to them.
- The usual aftercare issues such as GP letter, STI screening, ISVA re-contacting etc and also Hep B PEP if appropriate.
- Go through any concerns they have (bearing in mind the role of NHS111 for COVID-19 related matters).
Feedback to the team any ways that this process can be improved.
