An explainer
Executive summary
1. Pressure on the NHS has continued in recent months with emergency departments across the country experiencing the highest number of attendances for the month of May (2.24 million) – the third highest total since records began – but performance was nonetheless significantly improved on last year.
2. The high demand came after the NHS’s busiest winter ever and in a month which included three bank holiday weekends, where we typically see more people coming forward for urgent and emergency care, and significant disruption from industrial action. These pressures are also seen across primary and community care and mental health settings.
3. The most recent data shows that despite these pressures NHS staff are continuing to make progress on reducing the number of people waiting for care, with the average waiting time from the date of referral falling to 13.8 weeks.
4. By the end of April 2023 we had reduced the number of people waiting more than 78 weeks by over 90% from the peak. The number of patients waiting 65 weeks has fallen by 43% since the beginning of January 2023.
5. Occupancy in acute beds remains high with patient flow through hospitals a key challenge – this is due to a number of factors, including demand levels, industrial action and delays to patients being discharged, all impacting on bed capacity. Discharge challenges are often linked to capacity challenges outside of acute care, and the NHS is working with other organisations in health systems, including social care, to support people to leave hospital once they no longer need to be there.
6. The NHS has made progress on increasing support to those outside of hospital. Urgent Community Response helps avoid hospital admissions by providing urgent care to people in their homes. ICBs now have full coverage and the latest data shows that nationally 82% of patients were seen within the 2-hour standard, with every region exceeding or meeting the 70% target in the Planning Guidance.
7. In diagnostics, the NHS has increased community access and overall activity levels. More than 2 million checks and scans were carried out in April (2,016,200) with the overall waiting list for diagnostic appointments falling from 1.62 million to 1.56 million. Over the past 12 months 24.6 million checks and scans have been carried out. This has been supported by the NHS rolling out Community Diagnostics Centres, which have now delivered more than 4 million checks and tests.
8. The NHS continues to see high demand for cancer services. In the past year (May 2022- April 2023), over 2.8 million people were referred for urgent cancer checks by their GP, compared to over 2.6 million the previous year – a 7% increase. In the past 12 months, 327,312 people started treatment for cancer (May 2022- April 2023) compared to 321,144 in the year before.
9. Good progress continues to be made in activity levels in general practice. In April 2023, 24.8 million GP appointments took place, of which 561,000 were COVID-19 vaccinations.
Elective recovery
The NHS has made significant progress in reducing the number of people waiting the longest for care. In April 2023, 244,079 patients started admitted treatment – which is 7,905 (3.4%) more than the same month last year.[1]
This is despite operating in a very challenging environment with levels of demand continuing to fluctuate and ongoing industrial action having an inevitable impact on planned care.
As per the ambitions set out in the elective recovery plan, the aim is to virtually eliminate waits of over 65 weeks by March 2024.
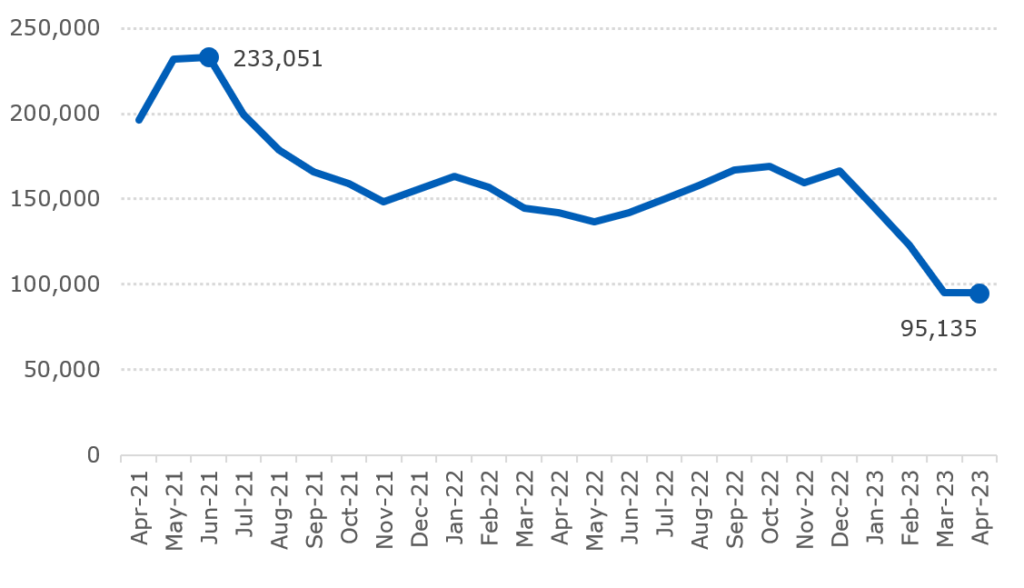
In April, 95,135 were waiting more than 65 weeks. This is down from a peak of 233,051 in June 2021 and is a reduction of more than 70,000 (43%) since the beginning of January 2023.
65 week waits
Waiting times for elective treatment have also fallen – the average waiting time is now 13.8 weeks. This is down from an average wait of 14.6 weeks in January 2023.
Four in five people who are waiting for treatment do not require an admission to hospital. Instead, they require some combination of outpatient care and diagnostic tests. The NHS completes over 100 million outpatient appointments every year, around 65 million of which are follow ups. The NHS is working to reduce the time people wait for an outpatient appointment by changing the way we deliver outpatient services and making greater use of technology.
Patients are being given more control to book their follow-up care, as and when they need it. Around 1 million outpatient attendances have been moved or discharged to a patient initiated follow up pathway – providing patients with more choice.
There is also a renewed focus on reducing reliance on low value follow up appointments where it is appropriate and safe to do so, freeing up time and capacity so patients receive the care they need, when they need it.
Urgent and emergency care
The NHS’s delivery plan for recovering urgent and emergency care (UEC) services sets out two clear ambitions for improving patient flow throughout the pathway.
The first target is to admit, transfer or discharge 76% of patients in emergency departments within four hours of arrival by March 2024. The second is to improve ambulance response times for category 2 incidents to an average of 30 minutes over 2023/24.
Meeting these ambitions will help patients get the care they need more quickly, providing the foundations for recovery and improvement across UEC services. Progress may vary through the year because at times our UEC services will be affected by levels of demand, seasonality, challenges with discharge, and industrial action.
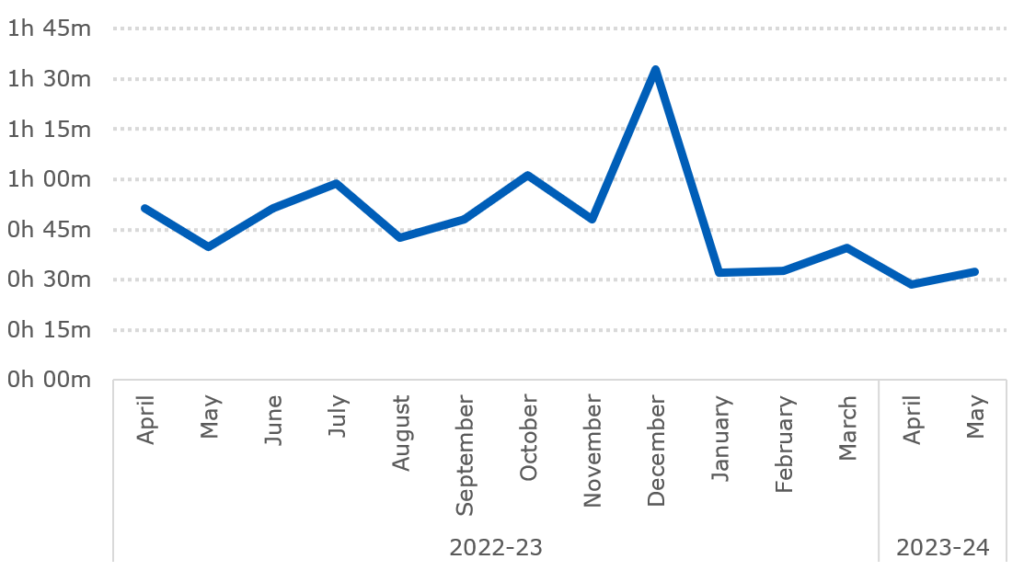
The average ambulance response time for a category 2 call was 32 minutes and 24 seconds, a faster response of 7 minutes and 30 seconds compared to the same time last year.[2] This was with 777,521 calls to 999 answered – 6% more per day than last month. Of these, 52% of incidents were conveyed to the emergency department, maintaining the reduced proportion of incidents conveyed compared to pre-pandemic.
Category 2 response times
74% of patients attending A&E were admitted, transferred or discharged within 4 hours[3] in May 2023. This was for 2,240,070 attendances in A&Es across England – an average of 72,260 a day, 10% more than last month.
Despite a month of increased pressure and further industrial action, performance is improving when compared to data from the same time period last year, showing the NHS continues to make headway towards recovering UEC services.
Cancer
Demand for cancer services continued at record levels in March with the number of urgent suspected cancer referrals at 122% of pre-pandemic levels. To meet high demand, treatment is also at record levels, and there has been a reduction in the 62-day cancer backlog as a result.
Over 327,000 people received treatment for cancer over the last year between May 2022 and April 2023 – the highest year on record, and up by more than 14,000 on the same period pre-pandemic.
GPs have been referring people for urgent cancer checks in record numbers since March 2021. Since then, NHS staff have seen over 810,000 more people than in the same period prior to the pandemic. The increase in referrals has contributed to the NHS diagnosing more cancer at an early stage than ever before.
Early diagnosis rates have risen for the first time in a decade. Survival is also at an all-time high. In 2023, the Annals of Oncology published findings showing that cancer deaths are around 10% lower in the UK compared to just 5 years ago.
The NHS is working hard to keep up with the increase in demand. It has been accelerating the installation of new diagnostic capacity, much of it in Community Diagnostic Centres. The NHS has already reduced the backlog by 12,000 people since the peak last summer, and despite the recent seasonal increase, NHS staff remain focused on making sure that the people who are seen first are those who have been waiting the longest or who need care the most urgently.
Notes
[1] 236,174 patients started admitted treatment in April 2022.
[2] The average response time in May 2022 for category 2 calls was 39 minutes and 54 seconds.
[3] 72.8% of patients attending A&E were admitted, transferred or discharged within 4 hours in May 2022.

