The purpose of this guide is to give information about a whole genome sequencing (WGS) test which is being offered to your child as part of diagnosis for cancer, suspected cancer and non-cancerous (benign) tumours.
Information in this guide should be used to supplement professional advice specific to your circumstances. If you have any questions, it is important to ask your child’s medical team.
What is a genome?
Our bodies are made up of cells. Each cell contains genetic information that makes us all unique, and this is written in a code called DNA. This works like a computer programme that tells each cell in your body what to do and how to do it. Your genome is a complete set of these instructions.
Science has now developed enough for us to be able to read this DNA information to help our understanding of tumours and cancer.
Most tumours and cancer are caused by changes in the DNA coding within a person’s genome or individual cells. These changes can happen when a baby is first growing in the womb or later in life.
Sometimes they can be inherited and passed down through family members. These changes can mean a person has a greater risk of developing cancer.
What is whole genome sequencing?
Whole genome sequencing is a way of looking at and comparing your child’s background DNA information (known as germline) with that of the tumour or cancer cells (known as somatic). These can be different and can help us to understand more about your child’s specific diagnosis and treatment.
WGS is offered to all children and young people who have or may have cancer, suspected cancer, or non- cancerous tumours.
Why consider a whole genome sequencing test?
The results may help us to understand:
- why your child has developed their tumour or cancer
- what type of tumour or cancer your child has and check that they are on the correct treatment plan
- how WGS may be used in treatment planning for the future
- whether your child has a gene which might increase their risk of developing other cancers in the future
- whether other family members may have a greater risk of developing cancer.
Your child’s healthcare professional will explain what happens and you will all be able to ask questions before you decide whether or not you want to go ahead.
By using a WGS test, this extra information may help doctors to consider the treatment plan for your child. WGS is a new service and the impact it may have on treatment plans is still being explored.
Whether or not your child has a whole genome sequencing test, your child will continue to get the best possible treatment and care.
What happens in a whole genome sequencing test?
To do a whole genome sequencing (WGS) test, a doctor will take the following two samples from your child:
- Blood, saliva, or skin sample – this sample shows DNA information inherited from parents. This is called a ‘germline’ sample.
- A small piece of cancer or tumour tissue (or bone marrow in leukaemia patients) – this sample shows DNA information of the tumour or cancer which may be different to the background or inherited DNA information. This is called a ‘somatic’ sample.
Whenever possible, samples are used from tests that are already being carried out as part of your child’s diagnosis. If additional tests are required, these will be discussed with you before you decide whether to go ahead.
Both samples are collected and sent to a genetic laboratory for testing. Scientists will compare the two samples and look for any differences in DNA. This comparison may give more information about your child’s particular condition.
A guide to your child’s whole genome sequencing test
Accessible image text:
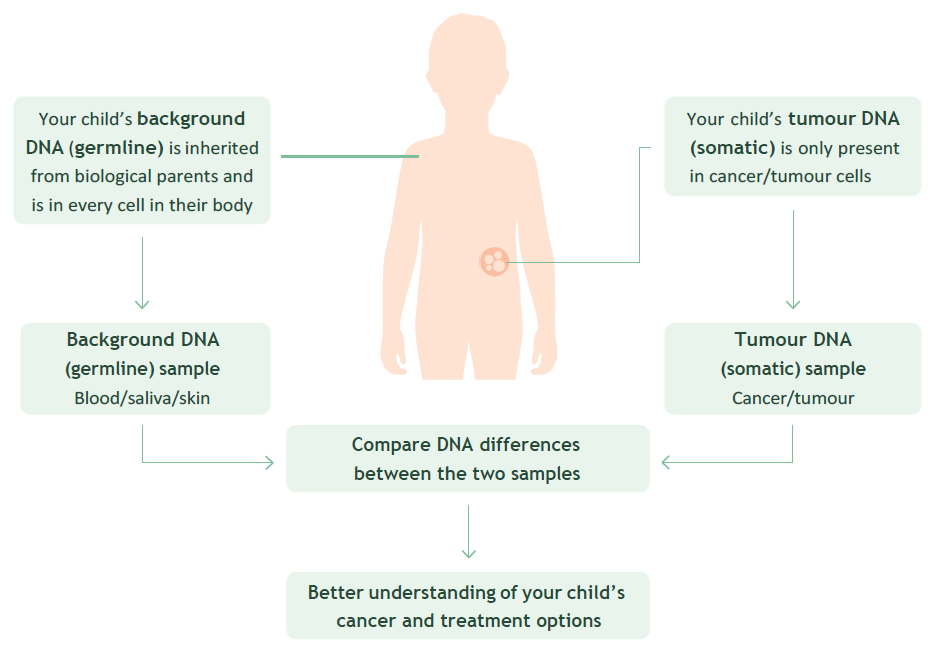
- Your child’s background DNA (germline) is inherited from biological parents and is in every cell in their body.
- Background DNA (germline) sample blood/saliva/skin.
- Compare DNA differences between the two samples.
- Better understanding of your child’s cancer and treatment options.
- Your child’s tumour DNA (somatic) is only present in cancer/tumour cells.
- Tumour DNA (somatic) sample cancer/tumour.
- Compare DNA differences between the two samples.
- Better understanding of your child’s cancer and treatment options.
Your child’s whole genome sequencing results
Once your child’s DNA has been looked at, the results are returned to your child’s healthcare professional who will share the results with you. This may take a few weeks. The result may give more information about your child’s condition and treatment.
This test is about identifying your child’s cancer or tumour type and linked genes so will not look for other unlinked cancer types that could occur in the future. It does not look for changes in DNA that may cause other health conditions.
There is a small chance it may also show whether your child has a higher risk of getting further cancers and if these risks may affect other family members.
In this case, you will be given the opportunity to discuss your results with a genetics specialist who will talk to you about your child’s results and how to manage any risks there may be for other family members. They will also help you to think about how to talk to your family members about your child’s result.
Important information about your child’s data
All data is kept securely and confidentially. Your child’s data is used in line with UK law and NHS policy. More information can be found at on the NHS England website: NHS England’s privacy notice.
Your child’s test data and results are stored in a secure database for the NHS Genomic Medicine Service – the part of the NHS that oversees whole genome sequencing. Only clinical, laboratory and healthcare staff linked to your child’s care and who have been authorised to do so can see this data.
You may withdraw your consent for your child’s data to be used or for you to be contacted at any point by visiting the Genomics England website: Participant resources.
Data use for insurance purposes
Insurance companies will not be given access to information about any predictive genetic test without explicit consent. When applying for an insurance policy, insurance companies may ask for medical and family history information. The information that is shared with insurance companies is regulated by a voluntary government code called the Code on Genetic Testing and Insurance.
Data use for research purposes
Health data donated by millions of other NHS patients has helped develop our understanding of diseases, new medicines and treatments. You will be given the option to contribute your child’s genomic and health data to a secure Research Library managed by Genomics England, so that approved researchers may access that data in a form that does not identify your child. If you choose to do this, you may be contacted in the future by someone in your child’s clinical team (or occasionally by Genomics England) to give you more information if anything has been found which might be relevant to your child’s health or that of your family, or if researchers identify a study that might be relevant to your child’s cancer. Data may be used to find new discoveries or to identify areas for new drug development.
Re-consent
Once your child reaches 16 years of age, and if you said yes to their data being added to the Research Library, they will be asked if they are happy for their data to continue to be used for research.
Further information
- Find out more about whole genome sequencing on the NHS.uk website: Genetic and genomic testing
- To find out more about how your child’s data can help research please visit the Genomics England website.