1. Introduction
This guidance details the clinical standards for the commissioning of anxiety management techniques for patients undergoing dental treatment in community and primary care settings. It does not apply to specialist services provided in secondary care or equivalent settings. It covers behavioural therapies, conscious sedation and referral for treatment under general anaesthesia.
- Section 2 focusses on anxiety management and the assessment of anxiety.
- Section 3 describes conscious sedation techniques appropriate to community and primary dental care settings.
- Section 4 outlines referral for treatment under general anaesthesia.
For ease of use, this guidance presents the three approaches to anxiety management (behavioural, conscious sedation and general anaesthesia) sequentially. However, it is important to remember that some patients require a combination of techniques or, perhaps, different techniques for different dental treatments. Behavioural techniques and conscious sedation must be viewed as complementary. Careful individual patient assessment for each treatment episode is crucial.
Tier 1 anxiety management refers to non-complex (ASA I/II) patients needing non-specialist dentistry. Tier 2 patients require more complex dental treatment and/or have a more complex medical history (ASA II+) where conscious sedation should be administered by a more experienced team.
2. Anxiety management
2.1 What is anxiety management?
The level of anxiety an individual experiences in relation to dental treatment is likely to vary from person to person, and according to the treatment performed. We can distinguish between ‘trait anxiety’ (the more enduring apprehension concerning dental treatment that a person generally feels when contemplating or engaging with dental treatment) and ‘state anxiety’ (the individual’s degree of concern at a specific point in time when faced with a particular aspect of dental treatment such as local anaesthetic injections). In terms of trait anxiety, the Adult Dental Health Survey suggests that approximately 51% report low levels of anxiety, 36% more moderate levels and 12% report trait anxiety at a level that could be considered ‘phobic’ (Hill 2012). The term ’phobia’ is reserved for an anxiety disorder comprising a marked and specific fear that is deemed excessive or unreasonable (APA 2000), and situations are ‘avoided where possible’ (WHO 1992). For state anxiety, it would generally be the case that more invasive treatments will provoke greater anxiety, and that individuals with higher levels of trait anxiety react with high levels of state anxiety in all situations. However, there may be some exceptions, such as dental injections which may be highly anxiety provoking for some individuals even in the absence of significant trait anxiety.
Approaches to anxiety management will largely focus on the reduction of state anxiety, with the goal of enabling the individual to engage in dental treatment and receive the care that they require with as much comfort as possible. However more intensive anxiety management approaches such as the use of pharmacological interventions and cognitive behavioural therapy (CBT) conducted by Tier 3 practitioners, are more likely to focus on reducing the level of trait anxiety, with the goal of allowing the individual to engage with primary care services at Tier levels 1 or 2.
Short-term and immediate anxiety management in dentistry includes approaches that can be adopted to provide necessary dental care, including needs assessment, treatment planning and treatment provision to an individual. However, accessing dental care is a life-long need, where long-term anxiety management approaches are required to support individuals in accessing dental care in primary care settings. This is where the rehabilitative benefits of behaviour management approaches, such as CBT and those built upon it, are fundamental in the consideration of patient pathways.
2.2 Complexity assessment – anxiety management
Assessment should comprise:
Assessment of trait anxiety. The Modified Dental Anxiety Scale (MDAS) provides a quick, reliable and robust measure to assess dental anxiety in adults. This five-point scale has specific items relating to different aspects of dental treatment; ranging from 5 to 25, scores 5-10 are mild, 10-18 are moderate, whilst scores of >19 or more are considered to be severely anxious/phobic of dental treatment.
Assessment of state anxiety triggers. The simplest form of assessment would be for clinicians to ask if there are any particular aspects of the treatment about which the patient is concerned. A more comprehensive approach would be to ask about specific triggers such as:
- The general dental environment (chair, waiting area, surgery, etc)
- Having an examination
- X-rays
- Local anaesthetic injections
- Use of the dental drill
- Scaling / polishing
- Extractions
- Determination of urgency of dental treatment need
- Determination of the health status of the patient (ASA status).
As outlined in the model of care, complexity will be a function of the level of trait anxiety and treatment urgency. Table 1 shows one suggested way of care provision on the basis of these assessments.
Table 1: A model of care by Tier level practitioners according to case complexity.
2.3 Illustrative patient journey – model of care
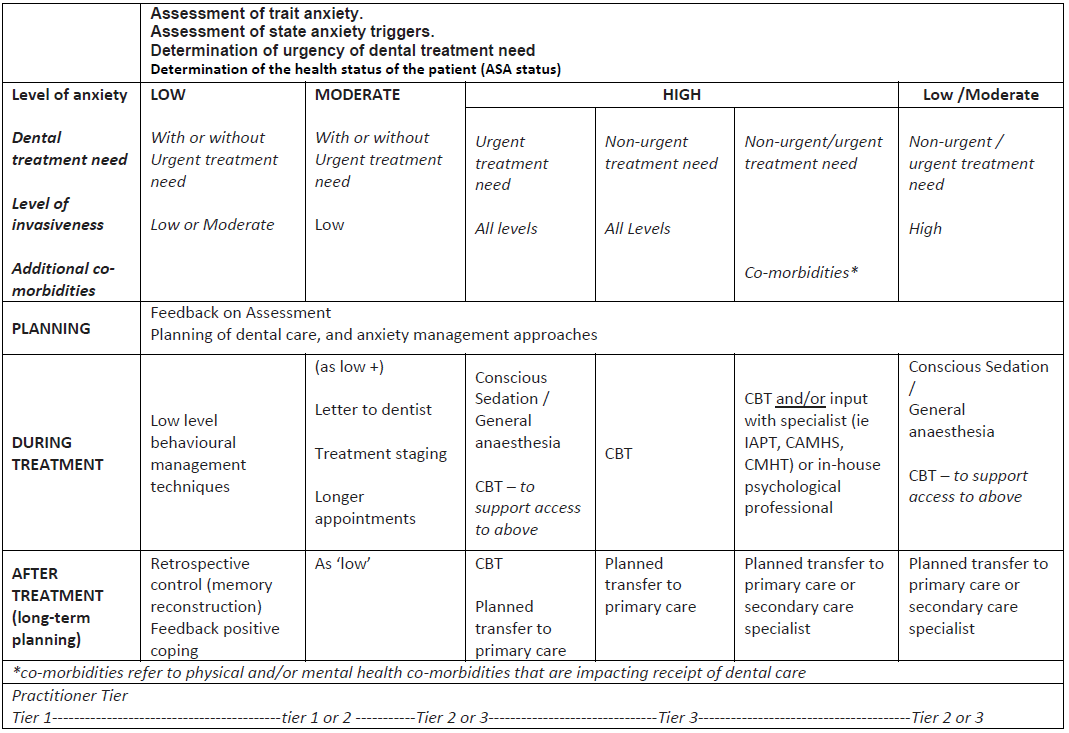
Table 2 shows a suggested model of care identifying where dental anxiety management techniques should be adopted according to the level of trait anxiety, the urgency and/or invasiveness of treatment need, and the psychological and physical health status (ASA) of the patient. It is envisaged that the greater the complexity of the patient need (both in terms of anxiety management and care needs) the greater the level of specialism required of the dental team.
Table 2: Model of dental anxiety management, according to dental anxiety, urgency of treatment care, invasiveness of treatment and any co-morbidities.
Low level dental anxiety management techniques – suitable for all patients, to be delivered by practitioners at all Tier levels.
There is a range of dental anxiety management techniques, typically taught to members of the dental team during pre-registration training. These include:
- Rapport building
- Environmental change
- Enhancing control
- Managing physiological awareness, including applied tension
- Retrospective control
- Feedback positive coping.
For further details, see appendix 1.
Advanced dental anxiety management techniques – suitable for patients with moderate and phobic levels of dental anxiety, high levels of invasive treatment and/or those with additional psychological and physical co-morbidities.
These include:
- Communication tools: Letter to the dentist
- Treatment staging
- Longer appointments
- Cognitive behavioural therapy (CBT).
For further details, see appendix 2.
2.4 Minimum training standards for behavioural techniques
Low level interventions: General Dental Council (GDC) registered members of the dental team with pre-registration training and experience in the low-level methods of dental anxiety management.
Advanced methods: Post-registration training and supervised practice in cognitive behavioural techniques for the management of dental phobia.
3. Conscious sedation
3.1 What is conscious sedation?
Conscious sedation is defined as:
‘A technique in which the use of a drug or drugs produces a state of depression of the central nervous system enabling treatment to be carried out, but during which verbal contact is maintained throughout the period of sedation. The drugs and techniques used to provide conscious sedation should carry a margin of safety wide enough to render loss of consciousness unlikely. The level of consciousness must be such that the patient remains conscious, retains protective reflexes, and is able to understand and respond to verbal commands’ (Academy of Medical Royal Colleges 2013, Inter-Collegiate Advisory Committee for Sedation in Dentistry 2020).
In the UK, the most commonly used dental conscious sedation techniques (titrated intravenous midazolam or titrated inhaled nitrous oxide and oxygen) have an excellent safety record. For many patients, conscious sedation combined with effective local anaesthesia is an acceptable alternative to general anaesthesia and makes treatment possible in primary care for a wider group of patients.
The clinical requirements in this guidance are aligned with reports on sedation from the Academy of Medical Royal Colleges (AoMRC), the Intercollegiate Advisory Committee for Sedation in Dentistry (IACSD) and the Scottish Dental Clinical Effectiveness Programmes.
Conscious sedation is important to the provision of high-quality dental care for some patients. It has relevance where dental treatment may be more advanced or complex, for individuals who experience disproportionate anxiety in relation to dental care or in the case of special care and paediatric dentistry where patients cannot co-operate with routine care.
All dental care must provide a needs assessment and treatment plan for each individual patient. This will include consideration of a range of behavioural (eg tell-show-do, Cognitive Behavioural Therapy, neuro-linguistic programming, hypnosis) and pharmacological options to offer the most appropriate treatment at each visit. It is important that sedation is regarded as part of a package of services that enable patients to access care. The package should not be sequential in nature but considered as a whole and the patient offered the most appropriate technique for their current treatment needs.
Valid consent is necessary for all patients receiving dental care under conscious sedation and this must be confirmed in writing. Consent should follow the principles set out in the GDC’s ‘Standards for the Dental Team’ and with regard to recent developments in case law (eg Montgomery v Lanarkshire Health Trust (2015)). The law now requires that a doctor, dentist or dental care professional must take ‘reasonable care to ensure that the patient is aware of any material risks involved in any recommended treatment, and of any reasonable alternative or variant treatments.’ A patient is entitled to decide the risks that they are willing to run (a decision which may be influenced by non-medical considerations).
3.2 Considerations for commissioning sedation
The provision of any services should be supported by a health needs assessment. A methodology for doing this is described in appendix 3.
Commissioners must carefully assess local referral rates and patterns of treatment services. This guide sets out the requirements for all referrals for dental treatment under sedation to go through a referral management system. By ensuring all referrals go through the referral management system it will be possible, over time, to better understand the need and volume of services to be commissioned to best meet the needs of the population.
Referral systems and patient assessment should include a valid and reliable assessment of sedation need. The Indicator of Sedation Need (IOSN) is one means of identifying, assessing and delivering appropriate sedation to patients. The premise of IOSN is that patients requiring sedation are not just dentally anxious but that the patient’s health, behaviour and physical and dental treatment complexity should also be considered.
IOSN comprises three elements:
- Modified dental anxiety scale (MDAS)
- medical and behavioural indicators
- dental treatment complexity.
Selecting the most appropriate conscious sedation technique for an individual patient must be based on a careful assessment of the:
- patient’s age and stage of development,
- degree of anxiety/phobia,
- medical and social histories,
- proposed dental.
The most straightforward technique which is likely to be effective, based on a robust patient assessment and on clinical need, is usually the best first choice. The administration of multiple sedation drugs is only indicated when more straightforward options have either failed, or when the sedationist is able to justify their use based on the outcome of the assessment visit or experience of previous treatment under sedation.
3.3 What will be provided in community and primary care settings
Conscious sedation in a primary care setting will be delivered in accordance with reports on sedation from the Academy of Medical Royal Colleges (AoMRC), the Intercollegiate Advisory Committee for Sedation in Dentistry (IACSD) and the Scottish Dental Clinical Effectiveness Programmes.
3.4 Clinical standards
The information provided below outlines the minimum clinical standards for all providers – appendix 4 contains a checklist.
All providers must only accept referrals which comply with referral management systems in place and that comply with referral minimum data sets. The minimum data set is likely to include some or all of the following items (SDCEP):
- A fully recorded medical history (including prescribed and non-prescribed drugs and any known allergies).
- ASA status
- A dental history
- A social history
- Any relevant conscious sedation and general anaesthetic history
- The dental treatment plan proposed
- Assessment of anxiety or sedation need and any tools used
- Any individual patient requirements
Providers must not accept patients who have self-referred or who have been referred outside of the agreed local referral management processes.
Ideally patients will be seen for assessment and consent prior to treatment; however, there may be occasions when it is clinically justified for patients to be assessed and treated in a single appointment (eg in the case of acute pain or sepsis). In instances where single appointment care is provided, commissioners should ensure that there is written evidence of the clinical justification for single appointment treatment.
Providers of conscious sedation must undertake training which includes supervised clinical experience in accordance with IACSD recommendations. A list of approved training providers is held by the Sedation Training Accreditation Committee (STAC) at the Faculty of Dental Surgery of the Royal College of Surgeons of England.
Each provider is required to complete sedation-related CPD in accordance with recommendations in the current IACSD Standards. An annual self-certified service compliance record is strongly advised (appendix 5).
3.5 Quality and outcome measures
In addition to the collection of quality and outcome measures, each provider will be expected to collect patient related outcome measures (PROMs) and patient related experience measures (PREMs) and report these to commissioners for the purpose of benchmarking
Clinical records should include:
- justification of need for sedation (eg MDAS, IOSN score) and audit of referral patterns
- satisfactory completion of planned dental
- treatment/recovery and discharge checks completed and recorded
- return for additional/emergency care relating to treatment provided at the last sedation appointment.
3.5.1 Patient reported outcome measures (PROMs)
- Was the sedation you received adequate for you to receive your dental treatment comfortably?
- Timely access
- Proximity.
3.5.2 Patient reported experience measures (PREMs)
- Thinking about the procedure you have had, were you provided with sufficient information prior to the procedure that enabled you to understand what would happen?
- Were you and your escort provided with sufficient information to be confident in looking after you in the recovery period since your sedation?
For CBT, the Treatment Evaluation Inventory (TEI) measure is designed to assess the patient’s perception of CBT-based treatment they have received both in terms of the benefit to them, and in terms of achieving a reduction on their dental fear. It is a 19-item scale which is scored by simply adding the total of all items.
4. Referral for general anaesthesia
All patients should be managed with the simplest and safest anxiety management technique which is considered likely to be successful.
For some anxious/phobic patients, including ‘pre-co-operative’ children, dental treatment may not be possible using behavioural and/or conscious sedation techniques alone. General anaesthesia may be also indicated if a large amount of dental treatment is required or because of medical problems and/or the complexity of the dental procedure.
Referrals for patients for dental treatment under general anaesthesia must indicate that the reason for referral and the referral process has been explained to the patient or their carers.
Careful consideration of all less restrictive anxiety management techniques, including behavioural therapies and conscious sedation must be undertaken before referring a patient for general anaesthesia. This is particularly important for those individuals who have been assessed as lacking the mental capacity to provide valid consent.
Referring practitioners must provide as much information as possible to specialist teams when they feel GA may be indicated. This should include any radiographs, information regarding the patient’s dental, medical and social history, the presence or suspicion of dental symptoms such as pain or infection as well as how the conditions are impacting a patient’s health and wellbeing. Details of treatment already carried out, the patient’s expectations and, when a dental examination has been possible, any treatment need identified.
The team offering dental treatment under general anaesthesia must establish the completeness of incoming referrals before a clinical assessment is arranged. They must also be able to demonstrate that they are appropriately trained and competent to carry out the treatment required
Where patients are referred for treatment under general anaesthesia, shared patient treatment plans and follow up responsibility between the patient’s general dental practitioner and specialist-led dental MCNs (where these are established), need to be in place (Geddis-Regan 2022, NHS England 2018, Royal College of Anaesthetists 2011).
Appendix 1
Low level dental anxiety management techniques – suitable for all patients, to be delivered by practitioners at all Tier levels.
Rapport building
Independent of which treatment modality is employed, the treatment of anxiety starts with establishing a good rapport. While essential for all treatment, the pharmacological effect of anxiolysis is enhanced and reinforced by a good relationship, empathy and tell-show-do.
Matching verbal and non-verbal communication is important. Research has shown that in the communication of feelings, only 7% is communication by words – the rest is shown in non-verbal language (55%) and tone (38%). The “4 A’s of Anxiety” provides a structure to consider – rather than well-intended reassurance, which has actually been found to be ineffective. Ask and Assess further demonstrate the importance of measuring anxiety, with Acknowledgment of concerns and offering suggestions to Address specific fears.
Environmental change
Dental instrument noises are often sirens to the anxious patient – consider what can be done to limit sound transmission from the dental surgery to the waiting area.
The smell of lavender has been shown to reduce adult anxiety on the day of treatment, although this is without altering beliefs of their global anxiety (Kritsidima 2010)
The types of images shown in the waiting area have been shown to reduce anxiety among children (Fox 2006), based upon theories of social learning and cognitive restructuring.
Enhancing control
The use of STOP signal is simple, yet so effective (Richardson 2009); it can also be modified to be used as a communication tool with a rising hand – whereby a resting hand is low anxiety and raising the hand before reaching a full STOP sign would indicate increasing levels, which can be monitored and recognised by dentist and nurse.
The perception of choice also affords some control for individuals, which has been shown to be effective in both medical and dental settings (Thompson 1981).
Managing physiological arousal
Providing techniques for individuals to manage their own anxiety is both empowering for the patient and time-saving for the clinician. Techniques to manage the uncomfortable physiology triggered by an anxiety response can be helpfully employed to reduce anxiety escalation.
Controlled breathing techniques (or diaphragmatic breathing) and Progressive Muscle Relaxation (PMR) have an established evidence base for anxiety reduction by reducing the sympathetic nervous system’s response before time would naturally dissipate anxiety. There are a number of techniques freely available online – and it is worth checking if individuals already engage in such exercises that they could try in the dental setting.
Applied Tension is an evidence-based technique (Ost 1987) to reduce the fainting response, by increasing heart rate and reducing the fall in blood pressure associated with the vaso-vagal response. This is particularly helpful for patients prone to fainting at the sight of blood, injections or injury.
Retrospective control
Enhancing control continues even after treatment has finished. Retrospective control is about helping patients understand what and why something happened – particularly if things don’t go to plan, or if a patient experiences discomfort or unexpected sensations. Reducing anxiety in this way has been associated with reduced experiences of pain post-operatively (Thompson 1981). This is also an important consideration if pharmacological approaches do not work as they intended; explaining possible reasons for this to the patient, may prevent them from misinterpreting the situation and developing catastrophic beliefs.
Feedback positive coping
Receiving praise, encouragement and labelling success and specifically asking the individual to identify these areas, after an anxiety-provoking event can support the creation of helpful memories – as opposed to dwelling on the ‘things that didn’t go well’. This technique conducted after treatment has been specifically demonstrated with children (Pickrell 2007).
Appendix 2
Advanced dental anxiety management techniques – suitable for patients with moderate and phobic levels of dental anxiety, high levels of invasive treatment and/or those with additional psychological and physical co-morbidities
Communication tools: Letter to the dentist
As part of increasing individual’s sense of control and involvement in their treatment, asking the patient to “write a letter to the dentist” in which they identify what would be helpful for them in coping with dental treatment, is a helpful way to contain patient information and put the control in the individual’s hands to let the dentist/dental team know what the triggers are, and what helps them cope. The document will require discussion with the team to ensure that they are comfortable engaging with the patient on each point.
Treatment staging
Consideration should be given to discussing whether it is possible (and preferred by the patient) to stage treatments from those perceived as less invasive by the patient to those that are more invasive, allowing the patient and the dental team to build an ongoing relationship of support over a series of visits.
Longer appointments
For individuals with moderate anxiety (ie MDAS scores 10-18); providing appointments longer in duration would support efficacious employment of some low level behavioural management techniques, in order to reduce anxiety and deliver treatment. For either patients with moderate anxiety who require it, or for patients stepping from Tier 3 to Tier 2, or Tier 2 to Tier 1 services, initially longer appointment times would support individuals to receive dental care. The length of the appointment could be reduced over-time, as anxiety levels reduce with the provider; working towards standard appointment times.
Cognitive Behavioural Therapy (CBT)
The National Institute for Health and Clinical Excellence, advocate Cognitive Behavioural Therapy (CBT) for a range of psychological disorders, including specific phobia. The use of Cognitive Behavioural Therapy (CBT) for the long-term management of dental phobia has been well documented (Ost 2013) and has a strong evidence-base for both its efficacy (ie how well CBT interventions treat dental phobia (Kvale 2004, Wide Boman 2013) and its effectiveness (ie how well these CBT interventions work in “real-world” clinical settings (Kani 2015, Porritt 2016). In a publication in the Royal College of Surgeons (England) Faculty Dental Journal, the complementary use of CBT within a conscious sedation care pathway has been endorsed; in which conscious sedation is deemed to provide an excellent approach to deliver dental care to the anxious individual, with CBT providing the long-term cure of the anxiety itself.
CBT combines two traditional theoretical approaches of behaviour therapy and cognitive therapy, which help an individual learn new strategies to solve problems related to their thoughts and behaviour. Both cognitive and behavioural interventions have been shown to be successful in reducing dental anxiety and increase dental attendance (Kvale 2004, Wide Boman 2013). These positive effects have been shown to be maintained over time (Willumsen 2003).
CBT is a brief, short-term talking therapy with treatment typically lasting 6 to 10 sessions: usually around 1-hour in duration.
CBT-based interventions for dental phobia could be delivered by registered psychological professionals (ie psychologists and CBT therapists), or any specifically trained dental professional; this could be a dentist, dental hygienist/therapist, dental nurse – all of whom would require competence and training by a competent body, for example a University.
CBT can be provided to support individuals to directly access dental care and treatment with local anaesthesia, as well as support patients to access conscious sedation or general anaesthesia when anxiety is too great. The latter is likely to affect individuals whose anxiety is preventing access to conscious sedation treatment; this is the only exception when CBT would be offered if urgent treatment was identified.
CBT – for urgent treatment need; (stress inoculation)
For some individuals unable to access conscious sedation due to anxiety, some CBT-based sessions with a trained professional could support access to methods of conscious sedation.
CBT and/or mental health complexities
If mental health co-morbidities are impacting receipt of dental care, it is likely to be beyond the suitability of CBT delivered by trained dental professionals; and is not recommended. For patients with or without urgent dental need and high levels of dental phobia, with mental health co-morbidity, input with a specialist service (ie NHS talking therapies for anxiety and depression, children and adolescent mental health services (CAMHS), community mental health teams (CMHT)) or in-house registered psychological professional is advised. Referral pathways and liaison with specialist services are important for these patients.
Appendix 3
Methodology for an area Health Needs Assessment exploring sedation, and oral health of a population.
Health needs assessment is a systematic method for reviewing the health issues facing a population, leading to agreed priorities and resource allocation that will improve health and reduce inequalities.
Further details may be obtained from the Office for Health Improvement and Disparities.
Appendix 4
Minimum service specification for conscious sedation services.
Personnel
- All staff including dental care professionals must be trained and experienced in the provision of conscious sedation services and able to evidence this.
- Healthcare professionals have appropriate indemnity cover and provide evidence.
- All staff must be registered with the appropriate bodies and regulators.
- Clinician carrying out pre-sedation assessment has conscious sedation training and experience and can evidence this.
- Dentist providing operative treatment has the necessary knowledge to provide dental care under conscious sedation and is able to provide evidence of this.
- Sedationist has the appropriate training and experience in conscious sedation for dentistry and is able to provide appropriate evidence.
- Dental Nurse (second appropriate person) has training and experience in conscious sedation for dentistry and is able to provide evidence.
- Registered healthcare professional assisting with recovery has training and experience and is able to provide appropriate evidence.
- Evidence of age related Immediate Life Support (ILS) training or equivalent for all healthcare professionals in the sedation team.
- Evidence of appropriate CPD for all healthcare professionals in the sedation team (currently 12 hours in a five year cycle).
Premises
- Must be clinically fit for purpose and fulfil legislative and regulatory requirements (lighting, heating, ventilation, safe access).
- Waiting room, surgery and recovery room are of adequate size for treatment and management of emergencies.
- Must provide adequate access for emergency services.
- Patients must be able to recover either in the surgery or in a dedicated recovery room prior to discharge where there are no patients awaiting treatment.
- Privacy assured in surgery.
- Individual privacy assured in recovery area and where possible on exit from practice.
Sedation delivery and equipment
- Chair/trolley rated to the patient’s weight, that can be rapidly moved to a head down tilt position during treatment.
- Facilities for the appropriate storage and disposal of drugs.
- Equipment serviced regularly and in line with manufacturers recommendations.
- Active scavenging and ventilation appropriate to COSHH recommendations and Health and Safety Regulations (2002) if applicable.
- Inhalation sedation machine unable to deliver <30% oxygen.
- Cylinder in use and full cylinder back up on inhalation sedation machine.
- Adequate central gas supply and cylinder empty alarms or automated switchover.
- Full and in use cylinder markers used.
- Central gas supply storage safety compliant.
- Central gas supply regulators in date and serviced.
- Appropriate gas storage in line with current guidelines.
- Emergency oxygen supply available.
- Automatic External Defibrillator (AED) (charged and batteries in date) equipment available with age appropriate and in date pads.
- Selection of blood pressure cuff sizes available.
- Variety of sizes of full face masks.
- Emergency suction available.
- Yankauer suckers available.
- Continuous pulse oximeter (with audible alarm) for use prior to and during treatment under sedation. (Not necessary for inhalation sedation).
- Bag/valve/mask system for intermittent positive pressure ventilation (adult and/or paediatric as appropriate) with reservoir and tubing.
- Oro-pharyngeal and naso-pharyngeal airways available.
- Emergency equipment readily available.
Patient Information
Requirement (all documentation for patients must be content, age and capacity appropriate).
- Patient information about the range of anxiety management care options available.
- Patient information regarding the conscious sedation technique to be used.
- Written pre- and post-sedation instructions.
Appendix 5
Service Compliance – Conscious Sedation Self certified checklist (www.saad.org.uk).