1. Foreword
Safeguarding babies, children, young people, and adults at risk remains a fundamental responsibility for everyone working within the NHS and its statutory and non-statutory partners. Across all NHS providers, integrated care boards (ICBs), and NHS England, we continue to take our statutory safeguarding accountabilities and responsibilities with the utmost seriousness.
The 2024/25 (fourth edition) NHS England Safeguarding Accountability and Assurance Framework (SAAF) recognised the cross-cutting nature of safeguarding across both adults and children within NHS organisations and providers of NHS services. This 2026 SAAF (fifth edition) builds on that foundation, reinforcing our commitment to ensuring the safety, protection, and welfare of babies, children, young people, and adults – including the prevention of harm and upholding the dignity of the deceased.
In shaping this edition, we have drawn on findings and recommendations from recent Public Inquiries, numerous statutory safeguarding reviews, and key national publications, including the 10 Year Health Plan for England and the NHS England Operating Framework. This alignment broadens the scope of the SAAF as a commissioning assurance framework.
As we embrace new ways of working, the 2026 SAAF also reflects the strategic partnerships we maintain with cross-government colleagues, notably within the Department of Health and Social Care (DHSC), as well as the Department for Education, Home Office, and Ministry of Justice.
I would like to express my sincere thanks to all those who have contributed to the development of this revised SAAF, and to everyone who continues to work with dedication and professionalism to safeguard the health and wellbeing of those most at risk.
Duncan Burton
Chief Nursing Officer for England
2. Introduction/purpose
This Safeguarding accountability and assurance framework set outs the safeguarding roles and responsibilities of all individuals working in providers of NHS-funded care settings and NHS commissioning organisations. It aims to:
- identify and clarify how relationships between health and other systems work at both strategic and operational levels to safeguard babies, children, young people and adults under the care of the NHS at risk of abuse or neglect
- clearly set out the legal framework for safeguarding children and adults as it relates to the various NHS organisations, in order to support them in discharging their statutory duties and requirements to safeguard children and adults
- set out the principles, behaviours, expectations and ways of working that reinforce safeguarding as everyone’s responsibility, ensuring that the safety and wellbeing of all – including individuals and communities at increased risk or in vulnerable circumstances remain central to our work and at the heart of our approach
- promote equality by ensuring that health inequalities are addressed and are at the heart of NHS England, integrated care board (ICB) and provider values
- outline the ways in which NHS England Regional and National teams support integrated care boards (ICBs) accountability and leadership at local level, fostering effective place-based partnerships
- identify clear arrangements and processes to be used to support evidence-based practice and provide assurance at all levels, including NHS England Board, that safeguarding arrangements are in place and are effective
This framework aims to provide guidance and minimum standards but should not be seen as constraining the development of effective local safeguarding practice and arrangements, in line with the underlying legal duties.
Safeguarding responsibilities form part of the statutory functions of each organisation, and executive boards must ensure these are discharged effectively within agreed baseline funding. As NHS England guidance on the roles of ICBs and NHS England evolves between 2025 and 2027 to deliver the 10 Year Health Plan for England, some ICBs will undergo changes, including mergers and boundary adjustments. These changes must not compromise safeguarding arrangements, which should remain robust and aligned throughout any structural transition.
Throughout the development of this document, we:
- give due regard to eliminating discrimination, harassment and victimisation; advancing equality of opportunity; and fostering good relations between people who share a protected characteristic under the Equality Act 2010 and those who do not
- given regard to the need to reduce inequalities between patients in access to and the experience of and outcomes from healthcare services.
3. Safeguarding context, legislation and mandatory reporting
Safeguarding is firmly embedded within the core duties and statutory responsibilities of all organisations that commission and provide NHS services across the health system. However, there is an important distinction between providers’ responsibilities to deliver safe, high-quality care and commissioners’ responsibilities to assure the safety and effectiveness of the services they commission through contracts, performance management and oversight.
Responsibilities for safeguarding are enshrined in international and national legislation. Safeguarding for both children and adults has transformed in recent years with the introduction of new legislation, creating duties and responsibilities which need to be incorporated into the widening scope of NHS safeguarding practice.
Regardless of the developing context, all health organisations are required to adhere to the following arrangements and legislation:
Legislation, statutory and recommended guidance for all ages
- European Convention on Human Rights
- Mental Health Act 1983
- Human Rights Act 1998
- The Crime and Disorder Act 1998
- Female Genital Mutilation Act 2003
- Sexual Offences Act 2003
- Mental Capacity Act 2005
- UN Convention on the Rights of Persons with Disabilities 2006
- Equality Act 2010
- Children and Families Act 2014
- Modern Slavery Act 2015
- Serious Crime Act 2015
- NHS Constitution and Values (updated Jan 2021)
- Domestic Abuse Act 2021
- Multi-agency statutory guidance for dealing with forced marriage and multi-agency practice guidelines.
- Health and Care Act 2022
- Serious Violence Duty 2023
- Prevent Duty 2023
- Online Safety Act 2023
- Victims and Prisoners Act 2024
Safeguarding adults
- The Care Act 2014
- Care and Support Statutory Guidance- Section 14 Safeguarding
- Adult Safeguarding: Roles and Competencies for Health Care Staff 2024
Safeguarding children and young people
- United Nations Convention on the Rights of the Child 1989
- Children Act 1989 and Children Act 2004
- Promoting the Health of Looked After Children Statutory Guidance 2015
- Children and Social Work Act 2017
- Child Death Review – Statutory and Operational Guidance 2018
- Marriage and Civil Partnership (Minimum Age) Act 2022
- Working Together to Safeguarding Children 2023
- Safeguarding and child protection in the Children and Young People Secure Estate 2023
- Children Social Care Reforms
- Safeguarding children and young people and children and young people in care 2025
NHS England is responsible for ensuring that the health commissioning system as a whole is working effectively to safeguard and promote the welfare of children. It is also accountable for the services it directly commissions or delegates, as per paragraph 237 in Working Together, 2023.
Every NHS-funded organisation, and each individual employee, contractor, trainee, volunteer and healthcare professional working in the NHS, has a responsibility to ensure that the principles and duties of safeguarding children and adults are applied holistically, consistently and conscientiously. These principles and duties should extend to unborn children as per the Child Protection Information System, and deceased people as recommended in the Independent Inquiry into the issues raised by the David Fuller Phase 2 report. The wellbeing of children and adults remains at the heart of everything we do.
Local authorities have a general duty under section 17 of the Children Act 1989 to safeguard and promote the welfare of children within their area who are in need. This includes the assessment of need for children in specific groups such as young carers, children with disabilities and children who have parents in prison. Section 47 of the Children Act 1989 creates a specific duty for local authorities to make enquiries to determine whether a child is or is likely to suffer significant harm, and what action to take to safeguard and promote a child’s welfare.
NHS bodies and providers commissioned by NHS bodies to deliver services on its behalf, have a statutory duty to assist the local authority with their enquiries, and contribute to multi-agency assessments, safeguarding processes and reviews. This includes timely information sharing, participation in strategy discussions, and provision of health assessments or reports.
In supporting local authorities to safeguard children in their local area, section 11 of the Children Act 2004 provides a statutory duty for bodies, including NHS organisations and agencies and the independent sector, including NHS England, ICBs, NHS trusts, NHS foundation trusts and general practitioners, to ensure that they discharge their functions having regard to the need to safeguard and promote the welfare of children. This includes providers commissioned by NHS bodies to deliver services on its behalf.
Local authorities have a specific duty under section 42 of the Care Act 2014 to make, or cause to be made, enquiries, to identify whether an adult in their area is experiencing, or at risk of, abuse or neglect to determine what action should be taken and by whom to protect the individual. Local authorities also have a duty under section 44 of the Care Act 2014 to review any situation where there is a reasonable concern that an adult has been failed by safeguarding.
Section 6 of the Care Act 2014 places a specific duty on NHS bodies to co-operate with local authorities in their enquiries and activities relating to adults with care and support needs, and carers. This includes supporting the smooth transition of young people from children’s services to adult care and support services. NHS organisations (ICBs and trusts) are legally required to work in partnership with local authorities in delivering care and support, and ICBs must be statutory members of Safeguarding Adults Boards (SABs).
Health services and local authorities have specific responsibilities under the Mental Capacity Act 2005 (amended in 2019), including the day-to-day operation of the Deprivation of Liberty Safeguards for adults. The NHS must ensure that every deprivation of liberty relating to an individual’s care, treatment or placement is considered and managed in accordance with the law, and must work with the local authority, where necessary, to authorise any deprivation of liberty that is in the individual’s best interests.
The NHS takes a leading role in the following safeguarding programmes which impact adults and their children: female genital mutilation (FGM), domestic abuse, prevent, domestic homicide reviews, modern slavery and human trafficking (MSHT). While safeguarding against FGM is typically focused on individuals under 18, it is equally important to engage with adults, both to safeguard them directly and to help protect any children in their care.
Every NHS-funded organisation needs to ensure sufficient safeguarding leadership and delivery capacity is in place for them to fulfil their statutory duties. They should regularly review their arrangements to assure themselves that they are working effectively to meet their statutory responsibilities including those set out in the NHS England Safeguarding Commissioning Assurance Toolkits (Safeguarding-CAT) for ICBs and providers. The toolkits set out the minimum standard and are not intended to constrain the development of effective local safeguarding practice and arrangements, in line with the underlying legal duties.
Organisations need to co-operate and work together within new demographic footprints to seek common solutions to the changing context of safeguarding, and to develop the structural landscape to deliver the NHS operational planning guidance, NHS England operating framework and the 10 Year Health Plan for England.
4. Roles of national, regional and local safeguarding
The national safeguarding team and Regional Safeguarding Leads (RSLs), collectively known as NHS Safeguarding, work to prevent abuse, exploitation and neglect, and to improve safeguarding practice across the NHS, supporting positive health outcomes for victims and survivors in all communities.
At a national level, NHS Safeguarding leads on statutory safeguarding reforms, national negotiations, and provides an integrated governance model for safeguarding across health and partnerships. It also delivers consistent assurance at system level and develops safeguarding learning products.
All RSLs reporting to the Regional Director of Nursing with responsibility for Safeguarding and operating under the leadership of the Regional Chief Nurse, are responsible for implementing national standards at a local level, supporting regional assurance processes, and promoting best practice in alignment with the NHS England operating framework.
This allows each region to support improvement through their safeguarding commissioning assurance governance processes, whilst ensuring the following key objectives are met:
- the implementation of effective safeguarding assurance arrangements via schedule 32 of the NHS Standard Contract, the SAAF, the Safeguarding-CAT, (provider and commissioner) and the NHS Safeguarding Case Review Tracker. This will include:
- Child Protection-Information Sharing (CP-IS) systems
- NHS contribution to local safeguarding partnerships
- Prevent
- MSHT
- FGM
- domestic abuse guidance
- Mental capacity and deprivation of liberty
- Children in care health assessments
- ensure regional and national direct commissioning, specialised, health and justice and armed forces commissioning are also meeting SAAF requirements at national, regional and local levels
- learn lessons from cases where children or adults die or are seriously harmed under the care of the NHS including statutory death reviews with safeguarding recommendations, to ensure the learning is effectively disseminated across the NHS
- NHS Safeguarding will provide safeguarding leadership and advice, across the NHS, underpinned by contemporaneous evidence-based methodologies such as contextual safeguarding; trauma informed practice and strength-based approaches to safeguarding interventions
4.1 NHS national safeguarding team
The role of NHS England is set out in the NHS England operating framework. The 10 Year Health Plan for England builds upon this, emphasising the role in providing clear direction, enabling delivery, and empowering staff across England.
The national safeguarding team will underpin the NHS England operating framework via our NHS Safeguarding workplan, as below:
| Operational framework | How will it be achieved |
|---|---|
| Sets direction | Via NHS standard contract schedule 32, the SAAF, and the suite of National Safeguarding Steering Group (NSSG) statutory safeguarding protocols for ICBs Work with Department for Education (DfE), Department of Health and Social Care (DHSC), the Home Office and Ministry of Justice to provide support in their development of safeguarding related statute and policy |
| Allocates resources | Via budgeting, commissioning and ICB offer, and via regional management teams. |
| Ensures accountability through the NSSG, the forum that provides assurance to the Executive Quality Group, quality committees and the NHS England Board | Via SAAF, the Safeguarding-CAT using the NHS Safeguarding Integrated Data Dashboard (NHS SIDD) and thematic audits NSSG leads the assurance of the NHS safeguarding system and offers strategic leadership for safeguarding and quality improvement across NHS England and the health economy |
| Supports and develops people | Via safeguarding clinical networks, communities of practice and the provision of learning material disseminated via networks and Futures. Through the collaborative development of the national All-Ages Safeguarding Mandatory and Statutory Learning (MaSL) and other thematic learning such as the MCA and Prevent |
| Mobilises expert networks | Via safeguarding clinical networks and clinical reference groups |
| Bring together expert knowledge to support service improvement | Via national safeguarding clinical networks |
| Support delivery of improved outcomes and provide benchmarks for services | Via the NHS SIDD and audit |
| Enable the spread of best practice | Via our networks, learning material, and the NHS Safeguarding Strategic Community of Practice |
| Manage relationships across national and professional bodies | Via liaising with cross-governmental departments to support the development of statute and policy, and with royal colleges to support the development of standards and competencies |
| Enable and support the development of systems and ICBs | Via the NHS Safeguarding Strategic Community of Practice, networks and protocols |
| Enables improvement | Via safeguarding clinical networks and learning events and material |
| Delivers services | Via the embedding of safeguarding across NHS programmes of work |
| Drives transformation | Via the NSSG, community of practice, networks, national and lead RSL topic leadership matrix, and regular RSL and regional chief nurses meetings |
4.2 The regional safeguarding team
The regional safeguarding team will support the NHS England operating framework through regional safeguarding work plans, which should align with their role in driving local improvement and performance, as outlined in the NHS England Model Region document (2025) (available via Futures).
| Operating framework for NHS England regions | How will it be delivered? Workplan/delivery plan functions |
|---|---|
| Act as the main voice to ICBs and the primary interaction between NHS England and systems | Liaison with the ICBs via: – chief nurses/clinical directors/deputies – head of safeguarding – designated professionals – named GP – regional safeguarding maternity leads/named midwives |
| Translate national strategy and policy to fit local/ pan-system circumstances, ensuring local health inequalities and priorities are addressed | Provide support, leadership and guidance on the development of NHS Safeguarding policies and procedures for safeguarding |
| Provide oversight of the performance of ICBs and providers and agree oversight arrangements for place-based systems and providers | Be the conduit for the evolving assurance of ICBs via: – the NHS Safeguarding heat maps – health’s role in multi-agency safeguarding arrangements for children – child death overview process – joint targeted area inspections – thematic reports from the National Child Safeguarding Review Panel – health’s role in SABs – review and analysis of data from the NHS SIDD |
| Develop leadership within ICBs and providers | Establish regional safeguarding networks, clinical groups and communities of practice as agreed within the region. Ensure all providers of health services and system leaders are engaged in arrangements for safeguarding babies, children, young people, and adults |
| Within national frameworks, determine the ‘how’ of delivery to achieve outcomes and expectations to reflect local populations, workforce, service structures and digital capabilities | Provide support to safeguarding improvements in the integrated care partnership (ICP) space. Delivered via regional safeguarding governance architecture, relationships and one-to-ones and communications |
| Develop mechanisms for systematically collating and sharing good practice and lessons learnt | Provide a lead RSL function within the NHS Safeguarding statutory functions providing leadership, support and guidance with the national safeguarding team. Support systems in making improvements via the application of learning lessons from statutory reviews |
| Manage regional level relationships including regional government | Provide performance oversight of any ICB or provider defined as meeting the criteria for intensive support by the NHS Performance Assessment Framework, where safeguarding is identified as a key risk. Delivered as directed via regional directors, regional chief nursing officers and system quality review groups (see regional safeguarding and quality governance architecture) |
| Provide support to ICBs to enable delivery | Collaborate with ICBs to escalate significant risks and issues which may have system-wide impact and require national resolution, to include learning from incidents such as: – child safeguarding practice reviews – domestic homicide reviews – safeguarding adult reviews – other local and regional safeguarding reviews |
4.3 The ICB safeguarding system
ICBs are statutory bodies. ICPs are statutory joint committees of ICBs and local authorities and do not exist as separate legal entities, albeit statute requires ICBs and local authorities to establish them as per the Local Government and Public Involvement in Health Act 2007 s116ZA, as inserted by the Health and care Act 2022.
The core role and function of ICBs is as strategic commissioners, as set out in the 10 Year Health Plan for England. As part of this role, ICBs assess the quality, performance and productivity of their commissioned and contracted services, as described in the Model ICB document (May 2025, available via Futures).
While NHS reforms are underway and guidance continues to evolve, primary legislation remains in force. Statutory duties therefore continue to sit with ICBs until any legislative changes are made.
The ICB chief executive officer, executive chief nurse, or the director-level executive with accountability for statutory safeguarding is responsible for the ICB’s commissioning assurance functions. This includes oversight of the delivery of the SAAF within the ICB and across all commissioned and contracted services.
The following programmes are the focus of an ICB-NHS Safeguarding protocol:
- CP-IS
- Child death overview process
- FGM
- Prevent
- MSHT
- Domestic abuse
- Domestic Homicide Reviews
- Managing concerns about missing people
The core principles of the executive accountability, including protecting the welfare and paramountcy of every child, and the principles of safeguarding adults at risk, will be upheld through the NHS SAAF.
The ICB executive chief nurse, or the director-level executive with accountability for statutory safeguarding, is likely to be the accountable member of the local strategic partnership structures:
- SABs
- multi-agency safeguarding children partnerships
- community safety partnerships
- violence reduction units (where in place)
- corporate parenting boards
- domestic abuse partnership boards
The ICB must ensure appropriate attendance at each partnership including at multi-agency risk assessment conferences.
In line with the statutory guidance set out in the Care Act 2014 and Working Together 2023, ICBs must employ sufficient designated professionals for safeguarding adults, children, children in care, as well as a named GP.
ICBs are required to act as joint and equal statutory safeguarding partners, as set out in the Children Act 2004 and as amended by the Children and Social Work Act 2017 . They must work with local authorities and the police within a multi-agency safeguarding children partnership to ensure that all functions are exercised to safeguard and promote the welfare of children in the area. Multi-agency safeguarding children partnerships are required to notify the Department for Education of their multi-agency safeguarding arrangements for children on an annual basis
Both SABs and multi-agency safeguarding children partnerships are required to publish an annual report outlining the arrangements made by safeguarding partners and evaluating their effectiveness.
While ICB directors can delegate responsibility for implementation of safeguarding practice across all ages, executive accountability for safeguarding cannot be delegated.
The ICB has accountability for strategic workforce planning. ICB safeguarding workforce plans should take into account the children, looked after children and adults safeguarding competencies and standards:
- Safeguarding children and young people and children and young people in care 2025
- Adult Safeguarding: Roles and Competencies for Health Care Staff | Royal College of Nursing
4.3.1 Section 11 audits
Section 11 of the Children Act 2004 creates a specific statutory duty for organisations to ensure their functions, and any services that they contract out to others, are discharged having regard to the need to safeguard and promote the welfare of children. This includes: NHS organisations and agencies and the independent sector, including NHS England, ICBs, NHS Trusts, NHS Foundation Trusts and general practitioners.
To monitor this, it is necessary for regular audits to be completed to ensure compliance. Local multi-agency Section 11 audits remain statutory and must be completed, with the Safeguarding-CAT, SAAF and NHS Standard Contract Schedule 32 acting as additional assurance tools. ICBs should collaborate with their local safeguarding partnerships to understand the specific local multi-agency audits.
4.4 NHS, health and care providers
All health providers, including provider collaboratives, are required under statute and regulation to have effective leadership structures and arrangements in place to safeguard and promote the welfare of children and adults at risk of harm and abuse in every service that they deliver.
Providers must demonstrate that safeguarding is embedded at every level in their organisation, with effective governance processes evident. Providers must assure themselves, the regulators, and their commissioners that safeguarding arrangements are robust and are working. These arrangements include:
- the contractual requirements as laid out in Schedule 32 of the NHS Standard Contract
- identification of a named nurse, named doctor and named midwife (if the organisation provides maternity services) for safeguarding children
- identification of a named nurse and named doctor for children in care
- identification of a named lead for adult safeguarding and a Mental Capacity Act (MCA) lead; this role should include the management of adult safeguarding allegations against staff. This could be a named professional from any relevant professional background
- safe recruitment practices and arrangements for dealing with allegations against staff
- provision of an executive lead for safeguarding children, adults at risk and Prevent
- an annual report for safeguarding children, adults and children in care to be submitted to the Trust board
- a suite of safeguarding policies and procedures that support local multi-agency safeguarding procedures
- effective training of all staff commensurate with their role and in accordance with the recommended intercollegiate safeguarding competencies. Where services are provided across the young people and young adult age ranges, that staff are competent in both child and adult safeguarding
- safeguarding must be included in induction programmes for all staff and volunteers
- providing effective safeguarding supervision arrangements for staff, commensurate to their role and function (including for named professionals)
- developing an organisational culture where all staff are aware of their personal responsibilities for safeguarding and information sharing
- developing and promoting a learning culture to ensure continuous improvement
- policies, arrangements and records, to ensure consent to care and treatment is obtained in line with legislation and guidance
Provider accountabilities and responsibilities must be considered in conjunction with professional accountabilities to the professional regulators.
5. Disclosure and barring service
The prevention of neglect, harm, abuse, exploitation and violence towards other staff, patients and members of the public is of paramount importance. Undertaking a Disclosure and Barring Service (DBS) is part of the safe recruitment processes within the NHS.
DBS is responsible for administering the government’s statutory scheme to help employers make safer recruitment decisions.
There are different levels of checks that disclose a range of different information contained within the Police National Computer and local police force information. The DBS provide guidance specifically for NHS roles: Role eligibility for DBS Checks | NHS Employers
6. Fit and proper persons tests
There are two ‘fit and proper’ persons tests that are separated within the health and social care regulations:
- Regulation 19 – which outlines the requirements for the fit and proper persons test for persons employed
- Regulation 5 – which outlines the requirements for directors to be fit and proper persons
7. Duty of candour
Safeguarding requires openness, advocacy, transparency and trust. The publication of the Francis Inquiry report recommended that a statutory duty of candour should be introduced for healthcare providers to be open with people when things go wrong; this duty is regulated by the Care Quality Commission (CQC).
The duty of candour is triggered by a “notifiable safety incident”, for any “unintended or unexpected incident that has occurred in respect of all service users during the provision of a regulated activity”.
The duty of candour may apply to safeguarding incidents that occur within healthcare providers where a clinical procedure or practice could have contributed to death, physical or psychological harm.
8. Information sharing
Robust information-sharing is at the heart of safe and effective safeguarding practice.
Information sharing is covered by legislation, principally the General Data Protection Regulations 2018 (GDPR) and the Data Protection Act 2018.
Practitioners must have due regard to the relevant data protection principles which allow them to share personal information. The GDPR 2018 and Data Protection Act 2018, place greater significance on organisations being transparent and accountable in their use of data and help organisations share information in a fair, proportionate and lawful way.
All organisations handling personal data need to have comprehensive and proportionate arrangements for collecting, storing, and sharing information. The GDPR 2018 and Data Protection Act 2018 do not prevent or limit the sharing of information for the purposes of keeping babies, including those on an unborn child protection plan , children, young people and adults safe.
Personal data may need to be shared to protect an individual from neglect or physical, mental or emotional harm, or to protect the well-being of a child under 18, or an adult defined as being “at risk” (Date Protection Act 2018). Sharing information to protect and promote the welfare of an unborn child must also be considered within health, and in the multi-agency safeguarding processes set out in Working Together, 2023. The Information Commissioner’s Office provides further guidance for safeguarding adults and children. Social Care Institute for Excellence(SCIE) provides further guidance for safeguarding adults.
The Child Protection-Information Sharing (CP-IS) programme assists the secure sharing of information between local authorities and health services to better protect children and young people who are known to social care because they are looked after or have a child protection plan, including an unborn baby protection plan.
CP-IS links IT systems across health and social care in England to help organisations share information securely. As it covers all local authorities in England, it is the only national register of social care status, and the only system to provide information when a child is out of area. ICBs are deploying CP-IS across a wider range of health providers during 2025-27.
9. Statutory and mandatory reviews
Statutory reviews are processes for learning and improvement and all health providers, including GPs, are required to provide and share information relevant to any statutory review process. All providers of NHS services that are asked to participate in a statutory review must do so.
ICBs, via the designated professionals, may support panel chairs where learning and improvement has wider implications and needs co-ordinated national action, and/or where there are obstacles to full NHS participation that require a range of relationship, contractual and professional influences.
9.1 Child safeguarding rapid reviews
As per Working together to safeguard children 2023, the purpose of rapid reviews for serious child safeguarding cases, at both local and national level is to identify improvements to be made to safeguard and promote the welfare of children.
Serious child safeguarding cases are those in which abuse, or neglect of a child is known or suspected and the child has died or been seriously harmed.
The safeguarding partners should promptly undertake a rapid review of the case in line with any guidance published by the Child Safeguarding Practice Review Panel. The aim of this rapid review is to enable safeguarding partners to:
- gather the facts about the case, as far as they can be established at the time
- discuss whether there is any immediate action needed to ensure children’s safety and share any learning appropriately
- consider the potential for identifying improvements to safeguard and promote the welfare of children
- decide what steps they should take next, including whether or not to undertake a child safeguarding practice review
9.2 Child safeguarding practice review
The responsibility for how the system learns the lessons from serious child safeguarding incidents lies with local multi-agency safeguarding children partnerships and at a national level, with the Child Safeguarding Practice Review Panel.
A child safeguarding practice review should be considered for serious child safeguarding cases where abuse or neglect of a child is known or suspected, and a child has died or been seriously harmed. This may include cases where a child has caused serious harm to someone else.
9.3 Child death review (CDR)
The Children Act 2004 requires ICBs and local authorities (child death review partners) to make local arrangements to undertake statutory CDR processes. The CDR process relies on inter-agency co-operation and information sharing.
These arrangements require the establishment of a child death overview panel, or equivalent, to review the deaths of all children (under the age of 18 years), regardless of cause of death, normally resident in the relevant local authority area; and if they consider it appropriate, the deaths in that area of non-resident children.
The review should then be carried out by a child death overview panel, on behalf of CDR partners, and should be conducted in accordance with Child Death Review: Statutory and Operational Guidance 2018 and Working Together to Safeguard Children 2023.
Multi-agency safeguarding children partnerships may consider undertaking a child safeguarding practice review following the death of a care leaver up to and including the age of 24, if they think learning can be gained.
9.4 Domestic homicide reviews (DHRs)
A DHR convened by the local community safety partnership is a multi-agency review of the circumstances in which the death of a person aged 16 or over has, or appears to have, resulted from violence, abuse or neglect by a person to whom they were related or with whom they were, or had been, in an intimate personal relationship, or a member of the same household as themselves.
ICBs are accountable to ensure lessons learned from any DHR are cascaded across the health system, and any commissioning/contractual measures with specific providers are implemented and learning is imbedded.
9.5 Safeguarding adults reviews (SARs)
SARs are required under the Care Act and convened by an SAB when an adult has died from, or experienced, serious abuse or neglect, and there is reasonable cause for concern about how agencies and service providers worked together to safeguard the person, as per the Safeguarding adults review quality markers.
ICBs are accountable to ensure lessons learned from any SAR are cascaded across the health system and any commissioning/contractual measures with specific providers are implemented, as part of local inter-agency safeguarding agreements.
9.6 Parallel investigations
At times, the safeguarding of children and/or adults in a health setting may feature in a Coroner’s Inquest or a wider multi-agency statutory review commissioned for other purposes: for example, a DHR or a Mental Health Homicide investigation, a Death in Custody Review or Learning Disability Mortality Review (LeDeR). In these circumstances, a separate safeguarding practice review may be deemed appropriate.
LeDeR is a service improvement programme which aims to improve care, reduce health inequalities, and prevent premature mortality of people with a learning disability and autistic people. Every adult (aged 18 and over), with a learning disability or with a diagnosis of autism who dies, is eligible for a LeDeR review. Learning from the deaths of children with a learning disability or autism are now managed through the Child Death Review process, and reported through the National Child Mortality Database.
The Patient Safety Incident Response Framework (PSIRF) may also be activated due to organisational incident management processes and investigations. Safeguarding teams should have a role in the oversight of PSIRF within their organisations.
Therefore, NHS organisations should be prepared to share information and co-operate with parallel practice review panels. Safeguarding leads have a role in ensuring that safeguarding is visible in these processes. Duplication of effort should be avoided where possible with each review informing the breadth of learning across the health and multi-agency partnerships.
10. Allegations against staff
Health organisations including NHS England must have a policy that includes the management and reporting of allegations and concerns about staff in line with the Care Act 2014 and the Children Act 2004. This policy should include the involvement of the organisational and professional regulators and the DBS as required.
10.1 Allegations against staff involving abuse or neglect – adults
The Care Act (2014) defines people in positions of trust (PiPoT) as “people who work in paid or unpaid capacity, including celebrities and people undertaking charitable duties with adults with care and support needs” (see Statutory Guidance 14.120 to 14.132).
It is a requirement of the Care Act 2014 Statutory Guidance that SABs should establish and agree a framework and process for any organisation to respond to allegations against “anyone who works, (in either a paid or an unpaid capacity) with adults with care and support needs”.
Where there is an allegation or concern that a member of staff in an ICB, primary care service, or a health provider has abused or neglected an adult in their personal or professional life, the designated professional for safeguarding adults in the ICB should be informed and organisational safeguarding and human resource processes followed.
10.2 Allegations involving harm or abuse of a child
Working together to safeguard children 2023 stipulates that information must be shared with the local authority designated officer (LADO) within one working day, where it is considered that a member of health staff poses a risk to children or might have committed a criminal offence against one or more children. The allegation may arise in the person’s home or professional life.
11. The regulation of safeguarding
CQC regulates compliance of the SAAF across healthcare – CQC safeguarding statement:
- working with other inspectorates such as Ofsted, HMI Probation, HMI Constabulary, HMI Prisons, and NHS England to review how health, education, police, probation and prison services work in partnership to help and protect people from harm
- working with local partners such as local Healthwatch, local authorities, the police and ICBs to share information about safeguarding people using services
Professional registrants must refer to their professional regulatory body:
- Safeguarding statement – GMC (gmc-uk.org)
- Our safeguarding policy – The Nursing and Midwifery Council (nmc.org.uk)
- Safeguarding Policy – Health and Care Professions Council (HCPC)
- Guidance on child protection and vulnerable adults (gdc-uk.org)
Other professional regulators will have safeguarding policies imbedded into their membership webpage.
12. Safeguarding governance – the role of the National Safeguarding Steering Group (NSSG)
NHS England’s safeguarding role is discharged through the Chief Nursing Officer (CNO) for England, who has a national safeguarding leadership role. The CNO is the lead board executive director for safeguarding and has several forums through which assurance and oversight is sought.
The NSSG is chaired by the Deputy Chief Nursing Officer for England – Professional and System Leadership, for NHS England. Through the NSSG, the Deputy Chief Nursing Officer for England leads the assurance of the NHS safeguarding system and offers strategic leadership for safeguarding and quality improvement across NHS England and the health economy
The NSSG gains assurance through NHS England’s national and regional governance and reporting frameworks, the NHS Safeguarding Integrated Data Dashboard (NHS SIDD) and feedback from NHS England safeguarding networks.
Membership of the NSSG includes representation from the national safeguarding team, regional safeguarding leadership, internal directorates, national safeguarding clinical networks and safeguarding partners such as the royal colleges and DHSC Office of Health Improvement and Disparities (OHID), and HM Government Arms-length bodies (ALBs).
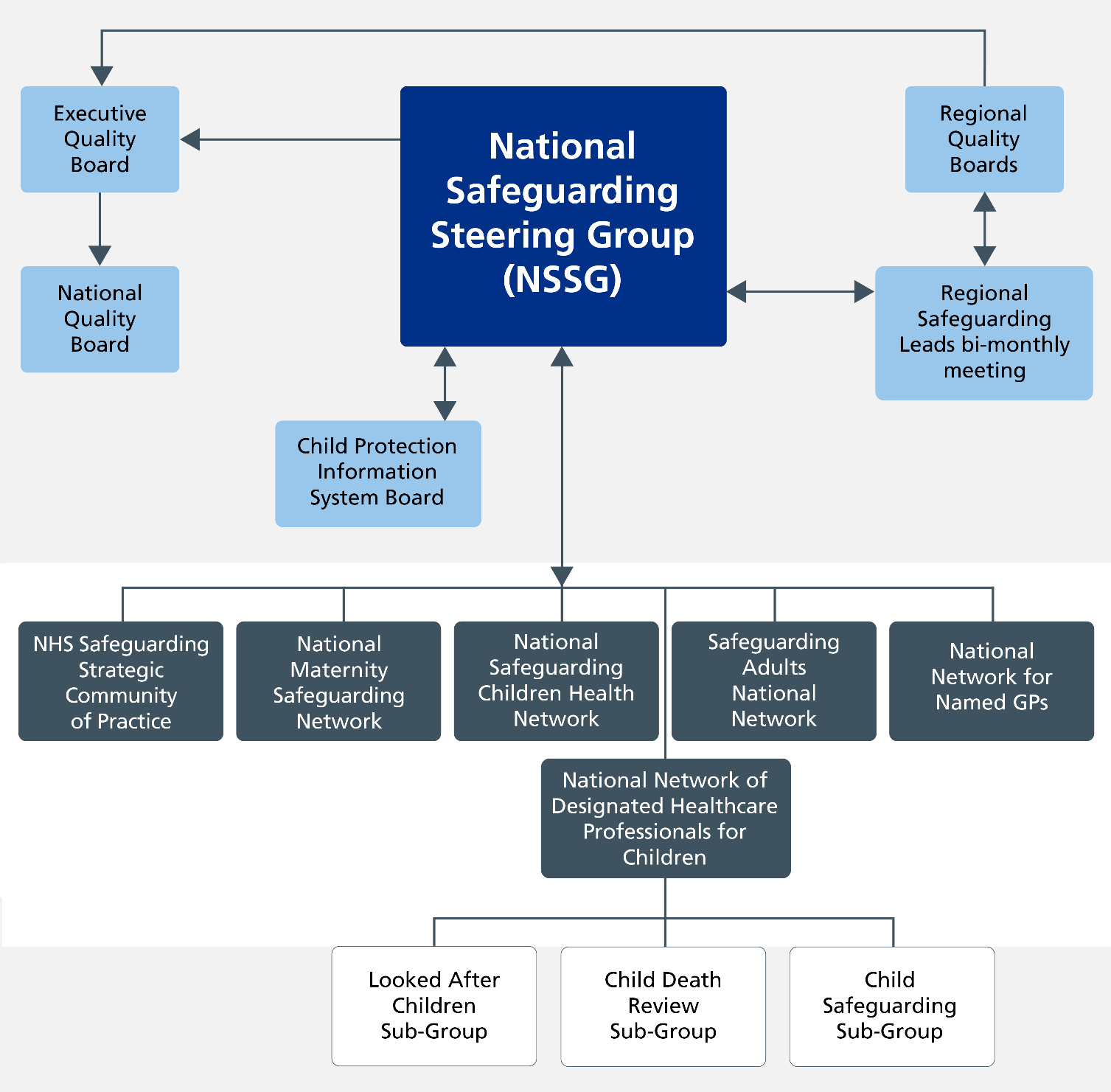
Figure 1: National Safeguarding Steering Group – safeguarding governance structure
Click here to read a detailed description of figure 1
The image shows a governance flowchart related to the National Safeguarding Steering Group (NSSG)
Here is a description of the flowchart:
At the top centre is a blue box labelled “National Safeguarding Steering Group (NSSG)”.
Directly above the National Safeguarding Steering Group box, there are two boxes:
On the left “Executive Quality Group”
On the right “Regional Quality Boards”
Below the National Safeguarding Steering Group box, there are four boxes:
On the left: “Child Protection Information System Board”
Second from the left: “National Safeguarding Adults Board”
Second from the right: “National Maternity Safeguarding Network”
On the right: “National Network for Named Safeguarding GPs”
Below these four boxes, there are additional boxes connected to them:
From “Child Protection Information System Board”: “NHS Safeguarding Strategic Community of Practice”
From “National Safeguarding Adults Board”: National Network for Looked After Children” “
From “National Maternity Safeguarding Network”: “National Network of Designated Healthcare Professionals”
From “National Network for Named Safeguarding GPs”: “Safeguarding Adults National Network”
At the bottom, there are three boxes connected to the boxes above.
On the left “National Forum for Children and Young People Safeguarding”
In the middle “NHS MCA Strategic Leadership Group”
On the right “Domestic Abuse and Serious Violence Policy Group”
The NSSG reports to the Executive Quality Group, in line with the NHS overseeing quality and performance framework of the National Quality Board. This supports oversight and alignment of NHS Safeguarding through the NHS Oversight Framework 2025/26.
As an organisation, NHS England must work with regulators to ensure there is a coherent system of quality oversight and regulation in place; one that is focused on improvement and enables warning signs, risks and concerns to be mitigated and managed as close to the point of care as possible.
NHS England oversees the delivery, performance, and improvement of both ICBs and providers. It works with ICBs to support system commissioning, contract quality management, and the development of best-practice care pathways, in line with NHS England’s National guidance on quality risk response and escalation in integrated care systems.
NHS England and ICBs will follow the NHS Performance Assessment Framework to manage ICBs and providers where safeguarding quality and performance is a consideration.
For independent providers of NHS services, ICBs are expected to ensure quality and performance through contractual levers and escalate concerns to NHS England regions. The oversight and assurance of some independent providers may be under the Independent Providers Risk Assessment Framework (IPRAF).
12.1 The national safeguarding networks
These networks form part of the NSSG, which commissions and funds their work to support the delivery of national safeguarding priorities.
12.1.1 National Network of Designated Healthcare Professionals (NNDHP)
The NNHDP is focused on child safeguarding. Designated professionals are experts and strategic leaders for safeguarding. As such they are a vital source of safeguarding advice and expertise for all relevant agencies and other organisations. The NNHDP have three sub-groups: Looked After Children, Child Safeguarding and Child Death Reviews.
12.1.2 Safeguarding Adults National Network (SANN)
The inclusive community of practice group for all matters adult safeguarding. SANN provides the national voice of adult safeguarding leads working for or on behalf of ICBs, NHS Trusts, independent health care, charities and third sector organisations from across England. Their role is to support NHS England in the strategic delivery of health outcomes from transition and adult safeguarding services across England.
12.1.3 National Maternity Safeguarding Network (NMSN)
The safeguarding group for anyone linked to perinatal and maternity safeguarding. The NMSN is a forum for regional, ICB and provider leaders in maternity safeguarding, to support the development and improvement of effective safeguarding practice across health systems. The network provides system leadership and oversight on maternity safeguarding and supports NHS England in the strategic delivery of safeguarding across England.
12.1.4 National Network of Named GPs (NNNGP)
The forum of named safeguarding GPs. The NNNGP serves as the representative body for named GPs for safeguarding in England. They represent the collective voice of named GPs for safeguarding in all matters related to safeguarding, and to actively contribute to the development of national policy, legislation, and guidance.
12.1.5 NHS Safeguarding Strategic Community of Practice
The NHS Safeguarding Strategic Community of Practice has been established to help ICBs understand and implement their executive accountabilities for the SAAF programmes.
12.1.6 National Safeguarding Children Health Network (NSCHN)
The NSCHN is a forum for those involved in safeguarding children in health services. This includes those working directly with babies, children, and young people as well as their parents and carers. The network provides a learning forum and the opportunity for all professionals to share and develop effective safeguarding practice in health.
13. Conclusion
The safeguarding of babies, children, young people and adults of all ages, is a fundamental obligation for everyone who works in the NHS and NHS funded healthcare. Safeguarding children and adults from abuse, exploitation or neglect must be kept constantly under review. Although the statutory duties for children and adults are set out in different legislation, all safeguarding should be person-centred and rights-based. Each person requires a unique safeguarding approach by the professional based on their circumstances and needs and the use of appropriate legal framework to protect them.
Fundamentally, every NHS organisation, and every individual working in the NHS, must ensure that the principles and duties of safeguarding adults and children are holistically, consistently and conscientiously applied: the needs of at-risk individuals and communities must remain central to all NHS safeguarding activity.
Partnership working is essential, and it is vital that executive, strategic and operational safeguarding leads, and all health practitioners continue to evolve relationships and work closely with colleagues across their local safeguarding system. This will help to develop ways of working that are collaborative, encourage constructive challenge, and enable learning in a sustainable and co-ordinated way.
The NHS is continuing to develop and improve safeguarding throughout the health services. The opportunities provided by the 10 Year Health Plan for England, new legislation, and learning from national reviews will ensure that we continue our focus on safeguarding our most vulnerable individuals and communities in a way that meets their evolving safeguarding needs.
Publication reference: PRN02452 (update to PRN01172)