Insights and learning from 24 trailblazer NHS organisations and integrated care systems
Summary
Purpose of this report
Between October 2021 and March 2022, NHS England supported 24 ‘trailblazer’ organisations and integrated care systems (ICSs) to engage with and use the revised Health and Wellbeing (HWB) Framework using a community of practice model.
This report is designed to share learning with others who are considering using the HWB Framework in their healthcare settings, to improve the health and wellbeing of their workforce and create a culture of wellbeing.
About the HWB Framework
The HWB Framework comprises a seven-element model that describes good workplace wellbeing in the NHS, and a toolkit that helps organisations to understand their needs, develop their strategy, and create an investment/implementation plan to help build a positive wellbeing culture. The NHS HWB Framework toolkit and supportive implementation resources can be found on our website.
Introducing the trailblazers
The trailblazers were spread across the seven NHS regions in England and comprise a mix of ICSs, clinical commissioning groups (CCGs) (pre-dissolution), primary care organisations, and ambulance trusts, acute, mental health, community and integrated care trusts.
How the HWB Framework was used
Trailblazers used the HWB Framework in various ways:
- Using the diagnostic tool to review wellbeing support and identify areas for development. Some focused on a few elements, others reviewed all seven.
- Hosting (virtual) workshops, meetings, or interviews to talk through the model with stakeholders, seek feedback for the diagnostic tool and/or co-design/plan next steps.
- Developing or refreshing a health and wellbeing strategy.
- Adapting the diagnostic tool so it could be used for quick self-assessment, particularly where multiple locations or partners were involved.
- Using the diagnostic tool to monitor progress over time, such as monthly or quarterly.
- Using the seven elements of the model to categorise health and wellbeing support in communications, on websites, and in newsletters.
- Promoting the benefits of the HWB Framework and how to use it, including giving presentations, buddying with another lead or having group meetings.
Benefits identified
NHS England worked with the trailblazers over a six-month period as a community of practice. In this time, most organisations had successfully engaged with/ completed the diagnostic phase of the toolkit; many had used the toolkit to develop/refresh their organisational HWB strategy, in line with the seven-element model.
Evaluation indicated that the short-term benefits reported from the HWB Framework included the following:
- Raising the profile of workforce wellbeing and its breadth, including with senior leaders or assurance groups.
- Building relationships across varied divisions and departments, appreciating that ‘health and wellbeing’ spans a broad scope of areas.
- Compiling evidence of the need to extend wellbeing support, to use when seeking funding from elsewhere eg senior leaders, CCGs, NHS charities, etc.
- Using data to inform decisions, including seeking feedback from the workforce and evaluating the support available.
- Gaining mutual support and reducing isolation of HWB leads in the organisation, by sharing experiences with other organisations.
Learning and top tips for others using the HWB Framework
Trailblazers suggested the following advice for other organisations and systems who are considering engaging with the HWB Framework:
- Engage with senior leadership.
- This is an important part of supporting culture change and sustainability, including resourcing.
- Set a realistic and structured timeline.
- The diagnostic tool does not need to be completed all at once. Organisations could do one section per week or month, but it is important to have a schedule in place, so the work is prioritised.
- One size doesn’t fit all; do what is right for your context.
- Focus on the areas that are most important or relevant to your organisation, rather than trying to do everything. The HWB Framework gives suggestions, not ‘must-dos’. Some things will be more relevant to some organisations/sectors than to others.
- If desired, adapt the diagnostic tool to be shorter and more visual.
- This can help engage a wider range of people and/or be used in meetings. Organisations can add questions or topics that are local priorities and simplify some of the wording in the diagnostic tool questions if circulating to stakeholders more widely.
- Your biggest source of data is your people.
- While workforce data is useful, bring people together to build a shared vision and ask them to assess how you are doing in relation to the seven elements. Use ongoing meetings and workshops to review the themes and plan next steps with your staff involved. It is less effective expecting a single lead to try to complete the tool alone or with minimal input from other people.
- Share good practice with other local organisations and help each other overcome challenges.
- This could be done through two leads buddying up and speaking each month, or by several leads from different organisations meeting.
- Remember that the diagnostic tool is just a tool rather than an end in itself.
- Aim to create an HWB strategy and practical action plan to guide investment and the changes you want, and review progress regularly so this is a living process that is part of business as usual.
- Repeat the diagnostic tool over time to track progress and change in creating your culture of wellbeing.
1. Introduction
1.1 The NHS HWB Framework
NHS England released a revised HWB Framework in 2021. This set of resources was intended to help NHS organisations create a sustainable wellbeing culture for their workforce and to pass on that wellbeing to patients. This built on the 2018 edition of the HWB Framework, which focused more on helping organisations reduce sickness absence.
The 2021 edition has seven focus areas or ‘elements’, and several sub-elements that have been identified as important for NHS organisations to address, in order to create their HWB strategy and instil a culture of wellbeing (Figure 1).
Figure 1: HWB Framework seven elements model
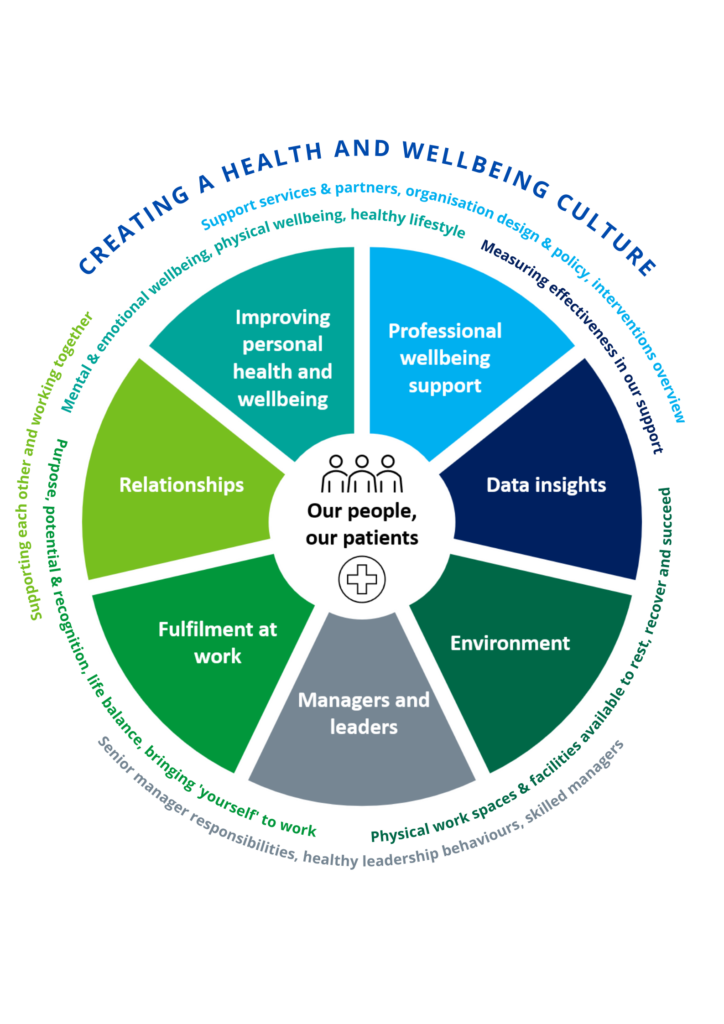
The HWB Framework toolkit consists of five resources to help organisations to create their HWB strategy and culture of wellbeing, including:
- Strategic overview
- Organisational HWB diagnostic tool
- Elements of health and wellbeing
- Implementation guide
- Case studies.
1.2 Introducing the trailblazers
Between October 2021 and March 2022, NHS England supported 24 trailblazer sites as a community of practice who could engage with, use and learn from the new HWB Framework toolkit and resources. Trailblazers were identified through direct expression of interest through regional HWB networks. They had to demonstrate they were in a good position to engage with the HWB Framework and had the backing of their organisation and senior leaders to do this. In return, NHS England supported them through this journey using a community of practice model.
Trailblazers were spread across all seven NHS regions in England and represented a range of organisations and systems including acute, mental health, ambulance and community trusts, ICSs, CCGs, a GP federation and a primary care network (Figure 2).
Figure 2: Map of trailblazer organisations
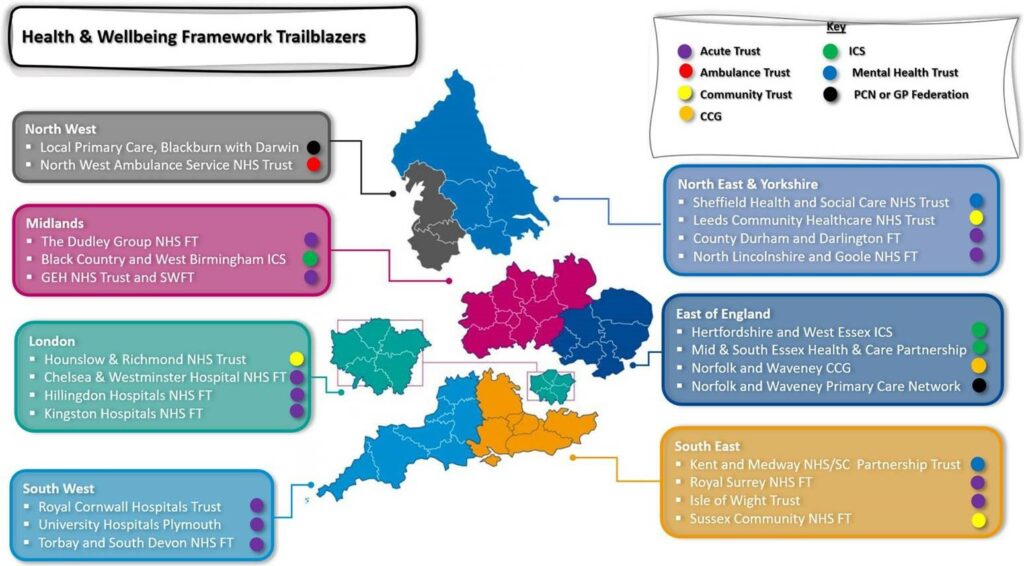
North West – 1. Local Primary Care, Blackburn with Darwin. 2. North West Ambulance Service NHS Trust. Midlands – 1. The Dudley Group NHS Foundation Trust. 2. Black Country and West Birmingham ICS. 3. GEH NHS Trust and SWFT.
London – 1. Hounslow and Richmond NHS Trust. 2. Chelsea and Westminster Hospital NHS FT. 3. Hillingdon Hospitals NHS FT. 4. Kingston Hospitals NHS FT.
South West – 1. Royal Cornwall Hospitals Trust. 2. University Hospitals Plymouth. 3. Torbay and South Devon NHS FT.
North East and Yorkshire – 1. Sheffield Health and Social Care NHS Trust. 2. Leeds Community Healthcare NHS Trust. 3. County Durham and Darlington FT. 4. North Lincolnshire and Goole NHS FT.
East of England – 1. Hertfordshire and West Essex ICS. 2. Mid and South Essex Health and Care Partnership. 3. Norfolk and Waveney (former CCG). 4. Norfolk and Waveney Primary Care Network.
South East – 1. Kent and Medway NHS/SC Partnership Trust. 2. Royal Surrey NHS FT. 3. Isle of Wight Trust. 4. Sussex Community NHS FT.
Each trailblazer committed to the following requirements:
- Assigning a lead/senior responsible officer to take forward the work.
- Working with senior leaders, such as the board, to gain organisational commitment.
- Working through the HWB Framework diagnostic tool to identify strengths and any areas for development.
- Developing an HWB strategy aligned with the elements of the HWB Framework.
- Sharing learning by providing a case study of the process and reporting on any barriers or key learning.
- Being an advocate of the HWB Framework with peers, including sharing experiences at monthly meetings and case studies to help others engage with the HWB Framework in the future.
Trailblazers were invited to attend monthly community of practice meetings throughout a six-month period to share progress, identify and find solutions to common challenges and provide peer support. NHS England asked for feedback about the community of practice sessions and adapted the content and format along the way. To supplement this, each trailblazer shared their experiences as they progressed through their journey with an independent team of evaluators to capture their personal learning.
The remainder of this document summarises the combined feedback from trailblazers about how they used the HWB Framework in this first six months, what they learnt and their suggestions to help NHS England and other organisations to ‘get started’ and implement the HWB Framework. The summary does not ‘evaluate’ trailblazers’ progress or the framework, but rather shares a ‘position in time’ around short-term learning.
The report describes the various ways that trailblazers used elements of the HWB Framework toolkit, followed by their perceptions and benefits from using it. It then summarises the advice trailblazers offered to other organisations interested in using the HWB Framework toolkit and suggestions for how it may evolve in the future.
One size does not fit all, and every trailblazer had a different experience of using the framework. Appreciating this, short stories explaining how each trailblazer used the framework are available separately.
2. Using the HWB Framework toolkit
During the six-month programme, all trailblazers developed plans and took steps to use the HWB Framework in the context of their healthcare organisation/system. Trailblazers began using the HWB Framework at a time of significant pressure on services and on health and wellbeing teams, including the emergence of the Omicron COVID-19 variant, winter pressures, and the pressures associated with the vaccination as a condition of employment.
This context is important, because it impacts on the extent to which trailblazers may have had capacity and motivation to take full advantage of the HWB Framework, and the ability of the organisations and their wider workforce to engage at the time.
2.1 Using the HWB Framework resources
Figure 3 shows the extent to which trailblazers had used the various resources in the framework and whether they found them useful. The diagnostic tool, elements of health and wellbeing and implementation guide documents were well regarded and perceived as most useful by trailblazer sites.
The resources people had used and found useful were similar regardless of whether trailblazer sites were integrated care systems or various types of healthcare trusts. However, primary care organisations were less likely to have engaged with the full suite of resources, potentially due to transferability to smaller healthcare organisation settings.
Representatives from primary care trailblazers emphasised that these were relatively small organisations, often without well-established wellbeing teams or initiatives, therefore they focused on using the diagnostic tool as a first step, as this was most useful for the stage they were at.
Figure 3: How the 24 trailblazers reported using the HWB Framework toolkit
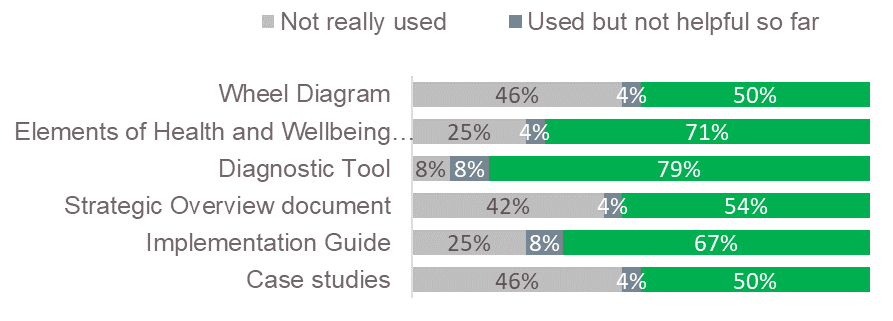
2.2 Using the diagnostic tool
Of the 24 trailblazer sites, 21 had applied the framework’s diagnostic tool to some extent during the first six months. Fifty-eight per cent had filled in the tool, with around half of these now planning ways to address any issues identified, and the other half implementing new initiatives because of using the Framework (Table 1).
Table 1: Stages of using the diagnostic tool
| Stage | % Trailblazers | Healthcare sector |
| Not started using in detail yet | 12% | 1 primary care 1 mental health 1 acute / integrated |
| Started using | 29% | 1 ICS 2 primary care 2 community services 2 acute / integrated |
| Completed tool | 8% | 2 acute / ambulance |
| Completed tool, planning initiatives | 25% | 2 ICS 4 acute |
| Completed tool, running new initiatives | 25% | 1 community services 1 mental health 4 acute / integrated |
Trailblazer sites took different approaches to using the diagnostic tool. The following offer common approaches, that could be considered by other healthcare organisations wishing to use the diagnostic tools:
- About half (46%) of trailblazers reviewed all seven elements in the diagnostic tool using a ‘light touch’ approach. Here, a single HWB lead either completed the tool themselves or co-ordinated completion, drawing on other stakeholders in the organisation for feedback. These groups answered all key lines of enquiry questions in the tool, usually basing this on leads’ opinions or readily available information.
- Over a third of trailblazers (37%) reviewed all seven elements in the diagnostic tool in detail. This included drawing on existing staff data (such as from the electronic staff record [ESR] and other workforce data sources), seeking feedback from a wide range of staff on how they perceived the organisation was doing in relation to the seven elements of HWB, and/or running workshops or meetings to discuss the diagnostic tool.
- About one in six trailblazers (17%) focused on between two and four elements in detail, as a way of making the tool more manageable.
Figure 4: Diagnostic tool use
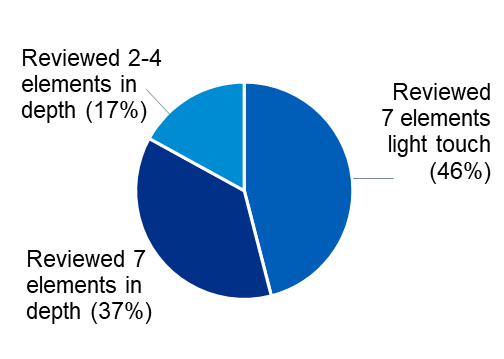
Around a third of trailblazers adapted the diagnostic tool to be shorter or more visual so it could be used for quick self-assessment, particularly where multiple locations or partner organisations were involved. These organisations tended to place all elements of interest on one spreadsheet tab or in a word document with a RAG-rating column. In some cases, these trailblazers removed lines of enquiry to concentrate on what they felt were the most pertinent areas.
Trailblazers held meetings or offered informal interviews to talk through the HWB Framework with stakeholders and seek feedback for use when completing the diagnostic tool. Some said the following approaches had worked particularly well:
- Informal conversations with staff and organisational stakeholders, where a lead asked them questions and used the feedback to complete the tool.
- The HWB lead completing a draft as a starting point for wider staff and stakeholders to contribute and review.
- Using the diagnostic tool as the focus of an existing health and wellbeing or assurance meeting, and then delegating the rest for completion by individuals outside the meeting.
- Running several workshops, bringing together frontline and managerial staff to review the tool and generate an action plan (generally the tool is too large to complete in one meeting).
| “We have explored the diagnostic tool as an assurance group, which was a really interesting conversation and helped us to think about what we do, could do, or do better based on the simple questions asked of us through this tool.” (Mental health trust) |
| “Using the diagnostic tool has bought us together to focus on wellbeing and any gaps we can improve on, this has come in handy with our ongoing review and it gives us data and insight into areas to focus on and look at our offer to staff… The HWB Framework seven element model allows us to group activity into categories which will help for planning and implementation and helps with explaining our vision to the staff and managers of the trust.” (Community trust representative) |
Some trailblazers gave one HWB lead the responsibility to undertake the diagnostic tool themselves, with limited ability to seek out information/evidence to complete this. This was reported to be a large burden for one person to lead such a complex task. These trailblazers tended to report less value from completing the diagnostic tool and raised concerns around their personal subjectivity of ratings, the time needed/capacity for one person to do this alone, and then the difficulties of gaining buy-in as others had not been engaged up front.
In contrast to this, trailblazers that engaged people to complete a simplified version of the diagnostic tool or extracted specific questions for stakeholders to complete reported good success, especially where there were follow-up group sessions to review the findings and plan next steps. These trailblazers were more likely to report wider benefits from this engaging approach, such as building relationships, sharing good practice or recognising a shared vision when collaborative approaches.
Trailblazers such as ICSs and organisations covering large geographical areas and many sites (such as ambulance services) needed to invest more time and resource in applying the diagnostic tool, due to the scale of the organisations and the desire to use a collaborative approach.
Individual acute, mental health and community trusts tended to report that it was more ‘straightforward’ to apply the diagnostic tool in their context. This was partly logistical, but also because the questions and focus areas were deemed to be relevant at the level of individual organisations.
However, one effective approach systems identified was to have each partner organisation undertake the diagnostic tool, then bring together the analysis of all partner organisations, and generate an ICS-wide diagnostic.
This helps to identify areas of good practice to share, and common areas of deficit where a system-wide approach to investing in health and wellbeing improvements may be useful; for example, if all partners rated managers and leaders lower, this can be a good starting point for system investment.
Many trailblazers were planning to, and/or had actively used the diagnostic tool to track progress over time, refreshing the tool as they began new initiatives or collated new data.
3. Perceived benefits
Table 2 illustrates the commonly reported benefits identified by trailblazer sites when using the HWB Framework toolkit:
Table 2: Commonly reported benefits of using the HWB Framework toolkit by trailblazer type
| ICS | NHS trusts | Primary care | |
| More focus on the breadth of health and wellbeing | ü | ü | ü |
| Set up or refreshed groups to discuss wellbeing | ü | ü | ü |
| Developed or refreshed health and wellbeing strategy or action plan | ü | ü | |
| Started new wellbeing initiatives | ü | ü | |
| New approaches to data review, benchmarking or reporting | ü | ü | ü |
| New ways to communicate about wellbeing initiatives | ü |
It was also identified that:
- 58% of trailblazers had used the diagnostic tool to highlight successes in health and wellbeing across the organisation
- 37% had shared a summary or the diagnostic tool with an assurance or governance group, raising the profile of and embedding HWB in existing governance structures
- 37% said they were helping other organisations use the framework, through informal and supportive conversations
- 25% had started new wellbeing support initiatives or refreshed existing initiatives.
3.1 Building relationships and culture change
Many trailblazers felt they had made progress towards building a positive wellbeing culture over the six-month programme, while appreciating that culture change takes time. Some of the reported benefits in creating this culture change included building relationships with organisational stakeholders, raising the profile of wellbeing among leadership teams and developing a shared vision or ways of working.
One of the most frequently reported benefits from using the HWB Framework was connecting to stakeholders within and across organisations. The role of the wellbeing guardian was also seen as critical to enabling this work and creating a culture of wellbeing, starting with the board.
| “The HWB Framework has improved my organisation’s awareness and connection with others to bring together an informal steering group for health and wellbeing and to work on implementing health and wellbeing into all areas of the organisation. To help with a culture change, health and wellbeing will be explored to implement into the service development plans and the directorate/division action plans.” (Acute trust representative) |
| “[Our] staff HWB engagement group has recently been refreshed, [and] now includes the board wellbeing guardian, staff members with lived experience of disability, trade union representatives, HWB champions and manager representation.” (Community trust representative) |
| “The diagnostic tool benchmarking exercise has highlighted variances in provision across the providers and provided an opportunity for shared learning and progression. For the first time, trust providers met to discuss the diagnostic tool, share experiences and agree on system and individual priorities. This approach was a huge success and further monthly meetings are planned with a topic for discussion agreed.” (ICS representative) |
| “The HWB Framework provided guidance with regards to effectively utilising our wellbeing guardian and through engaging with a wide range of stakeholders, our wellbeing guardian has championed our priorities which we will use to guide our focus to improve the health and wellbeing of our staff.” (Mental health trust representative) |
One of the main differences between the 2021 and 2018 editions of the HWB was a focus on embedding equality, diversity and inclusion (EDI) when thinking about workforce wellbeing. Many trailblazers mentioned working closely with EDI leads to feed into the diagnostic tool, and in some cases to undertake joint engagement work with staff or plan new initiatives.
Some reported that the HWB Framework had influenced them to think in detail about EDI in relation to wellbeing for the first time and/or that it was the first time that wellbeing and EDI leads had worked closely together.
Some trailblazers reported sharing their experiences with other local organisations about the benefits of the HWB Framework and how to use it, including giving presentations, buddying with others or having regular peer support meetings across a local area, system or region.
3.2 Creating a compelling and positive vision, and celebrating successes
Trailblazers reported using the results from the HWB diagnostic tool to celebrate successes, raise the profile of workforce wellbeing, and create a positive vision for their wellbeing culture, including gaining support and engagement with senior leaders and/or assurance groups.
| “We have been able to use the toolkit to celebrate the work we had achieved so far. It was helpful to see that we had already achieved a lot and the toolkit helped us to map our work against key themes.” (Ambulance or integrated trust representative) |
| “The new additions to the HWB framework ‘seven elements model’ [have] certainly been of benefit and aligns much closer with the culture we are wishing to promote. It has been easier to engage with staff.” (Trust representative) |
| “The HWB framework has highlighted the amazing work that is already happening/in progress and areas which could be improved upon, making it more transparent and readily accessible. It has enabled thought/consideration to ‘next steps’ and identified actions to take forward.” (Acute trust representative) |
Several Trailblazers reported that they had used results from the diagnostic tool to develop or refresh an existing HWB Strategy.
| “Participating as a trailblazer site and as a member of the community of practice has been extremely helpful in progressing a culture of health and wellbeing within the trust, culminating in the development of a strategy we are proud of and will be working to for the coming three years… With the framework’s focus on creating a culture of health and wellbeing, senior strategic leaders have recognised the role that wellbeing can play in ensuring it delivers our priorities and wellbeing has now been included as a key strategic workstream.” (Mental health trust representative) |
| “By taking part in the trailblazer it has allowed us to have a dedicated focus on developing our HWB strategy. We have accomplished a wealth of interventions over the last few months, and the framework has shone the light on areas that need a refocus. On the back of this we are now creating our new health and wellbeing website, which is focused on the new pillars, have created new reporting mechanisms for data and to ensure a fully integrated approach across a range of support services within the trust.” (Acute trust representative) |
3.3 Enhancing wellbeing support
A quarter of trailblazers reported using the diagnostic tool to evidence the need to enhance/develop HWB support services and offers and built their business case around this. This enabled them to approach senior leaders or charities for resourcing/funding.
Trailblazers also reporting using the HWB Framework to develop/test innovative HWB support offers. Examples of new initiatives set up as a direct result of using the HWB Framework included:
- promotional activities such as a new signposting website or newsletter
- data dashboards, reports or using data differently
- needs assessment survey or focus groups
- changes to physical environment
- healthy lifestyle activities
- wellbeing champions
- psychological debriefing
- health and wellbeing stakeholder group.
A key difference that was identified by trailblazers when comparing the new and previous editions of the HWB Framework, was the increased focus on preventative health and wellbeing interventions in the new edition. Trailblazers reported being more empowered to focus on preventative approaches and/or communicating the breadth of support available.
| “This highlighted that we needed to do some basic/foundation interventions to ‘warm’ staff up before focusing on some of the other areas. Supporting positive mindsets but also just bring staff together in organisation-wide activities so that they are more likely to engage when we move onto focused work.” (Primary care representative) |
| “We realised that, as a trust, our healthy lifestyle provision was fairly limited. In response, we have been exploring how we can use in-house members of staff to support with this. We have already implemented monthly smoking cessation sessions specifically for staff, promoted the use of our sleep team and have been increasing the communications surrounding the staff gym.” (Acute trust representative) |
3.4 Promoting existing support
Trailblazers often identified promotion of existing health and wellbeing support as an area for development and took steps to change this. Several also found it useful to categorise their support offers under the seven elements of the HWB Framework model. Trailblazers reported how it was useful to grow the wellbeing champion role and wellbeing conversations as part of creating a culture of wellbeing locally.
| “We have changed how we promote the health and wellbeing champion role. We have filmed two videos to explain the role and show what some teams are already doing. Four drop-in sessions have taken place to give staff the opportunity to find out more about the role if they are interested. The sessions were well attended, and most attendees signed up to the role following the session. More than 50 members of staff have signed up to become a champion.” (Acute trust representative) |
3.5 Using data over time
Many trailblazers reported that they were using the diagnostic tool to monitor progress over time, by updating it regularly. The diagnostic tool provides a measure of self-reported elements of a health and wellbeing culture, so tracking progress over time would allow organisations to monitor the extent to which they are perceiving changes in their wellbeing culture.
Trailblazers reported that using the HWB Framework had positively impacted how they were seeking feedback from their workforce about their needs and using data to evaluate existing offers and plan additional support, or scale and spread these.
| “To gather data for the diagnostic tool, we have also had to consider ways to increase engagement, and we have successfully established several ways of doing this – through joint initiatives with the EDI team, themed events around national awareness days such as International Women’s Day, through a mix of face-to-face and virtual work and through identifying existing meetings, training days and events where we can engage with staff to both highlight the support offer and gather soft intel.” (Acute trust representative) |
| “We trialled initiatives as part of the pilot, and subsequently evaluated these, which has led us to identify what changes we might need to make when upscaling initiatives to increase staff engagement and effectiveness of interventions. For example, we trialled psychological debriefings with [the intensive therapy unit] and [high dependency unit], and while feedback was good, uptake was poor. Through evaluation we were able to identify that staff were struggling to find both the time and mental capacity to engage, and we are now refining the intervention so that this happens as part of existing ward meetings, huddles, etc.” (Acute trust representative) |
4. Enabling factors
4.1 Main factors
Trailblazers were unanimous in reporting that the HWB Framework seven element model was helpful and contained valuable elements that promoted a wellbeing culture. Those who had used the 2018 edition of the HWB Framework said that they welcomed the wider breadth and more holistic approach to HWB within the updated edition and the reduction in focus on sickness absence as a core driver.
Trailblazers reported wider enabling factors that facilitated use of the HWB Framework were:
- ringfenced time/capacity to spend using the framework, including a named HWB lead/team scheduling activities maintain momentum
- leadership engagement, which was important to ensure ringfenced time, but also agreeing actions and potentially resourcing for priorities identified for development
- taking a team approach, such as having working groups or reviewing actions in meetings, rather than being only the remit of a single HWB lead
- opportunities to share ideas with people from other organisations, either locally or nationally, through meetings or via case stories
- visual elements of the Framework, such as the wheel diagram
- access to data including generating new data by engaging staff within their organisation to share their perceptions against the seven elements.
Connection and relationship building as part of the community of practice methodology working with NHS England was also reported as one of the key benefits. Trailblazers reported that being a part of the trailblazer community of practice provided opportunities to network and learn from others. In some cases, it also helped to validate and give status to wellbeing work within organisations. Many people also said that having an hour or two each month to meet with other like-minded people helped them feel motivated and less alone.
4.2 Things to consider
While the HWB Framework toolkit use was reported positively, trailblazers also reported things to consider when starting out on the journey of using the toolkit. Many of them reported that the diagnostic tool and accompanying documentation could initially be overwhelming in breadth and depth for those new to workforce health and wellbeing. This is why many of them successfully adapted the tools for local use, such as creating simplified versions of the diagnostic tool when engaging their staff.
| “Our initial observation was that it all felt very overwhelming to complete – mainly due to its size and level of detail. However, once we adapted the tools and our approach and we were able to make this more manageable and more suited to us.” (Ambulance or integrated trust representative) |
| “The HWB Framework is well structured and comprehensive but remains daunting in sheer volume. We are mainly using this with small, private sector practices that don’t have the capacity to engage in this fully.” (Primary care representative) |
Trailblazers reported that the toolkit was valuable and evidence-based, yet the sheer size of the ask to engage with best practice in the toolkit meant that busy or smaller-resourced teams may have less capacity to engage. There was a perception that it could be burdensome or time-consuming.
Trailblazers suggested that it would be useful to use short visual documents as a way into the HWB Framework to get people interested (eg a two-page document with visuals, or separate two-page documents about each element of the wheel). They also suggested short (5-10 min) videos/animations introducing the purpose, tool(s) and each of the seven elements.
Around a third of trailblazers made their own shortened version of the diagnostic tool (eg using the RAG-rating column in each tab only). Sites reported that this was more manageable than the full spreadsheet. These trailblazers said that having the full spreadsheet was useful strategically for them as a HWB team, but not practical to complete quickly, especially where multiple organisations or departments were involved. Some areas used their shortened version monthly or quarterly as a progress update.
Trailblazers also suggested that it is important to use the framework toolkit content flexibly and adapt it to local context, as we are working in a ‘one size does not fit all’ complex healthcare environment. For example, several of the lines of enquiry in the diagnostic tool were reported to be more relevant to NHS trusts than CCGs, primary care networks, ambulance services and ICSs.
This may be particularly important in the changing context of integrated care systems and the driver to involve a much wider range of stakeholders in planning, managing and supporting the workforce. However, trailblazers appreciated the ‘not applicable’ rating in the diagnostic tool to get around this, and enable them to apply it to their local context.
| “We included non-NHS partners. Some people thought this was an ‘NHS Framework’ so it may not apply to them, but we found that councils and other partners were happy to engage. This helped to paint a more complete picture of workforce wellbeing across our whole system.” (ICS representative) |
Trailblazers also highlighted that there are limited budgets and capacity to take forward health and wellbeing work, and this is something to be mindful of. Creating a compelling business case to secure organisational investment in HWB is essential and the diagnostic phase gives the data to inform this business case.
| “Many of the suggestions within the HWB framework were brilliant; however, in reality many will be very difficult to implement due to budgetary limitations. We have to become better at business planning to gain the resource we need.” (Acute trust representative) |
5. Sharing the learning and ‘top tips’ from trailblazers
This section summarises the ‘top tips’ for other organisations wishing to engage with using the HWB Framework, from the learning across trailblazer sites. In summary, the most common advice was:
5.1 Engage to co-design a wellbeing cultural change
- Get senior leadership support from the outset, as the HWB Framework is about culture change. If leaders are involved from the start, they may expect reports on progress and be more likely to resource identified areas for development. Building into existing governance processes can work well, including working with the board wellbeing guardian and the people governance team.
- Involve a wide range of stakeholders in completing the diagnostic tool and designing your strategy and interventions, rather than asking a single person/HWB lead to try to complete it alone or with minimal input. Engaging with staff and wider stakeholders across an organisation or system is crucial, so using the HWB Framework is not seen as something developed by the organisation, by the organisation, rather than ‘top down’.
5.2 Apply project management methodology
- Set a realistic but structured timeline to complete the diagnostic tool, implement findings and seek out as much evidence as you can from a variety of sources. Achieve this by taking small steps and the diagnostic tool does not need to be completed all at once. Organisations could do one section per week or month, but having the time scheduled in and deadlines is useful to maintain momentum.
- Be driven by your local need and focus on areas that are most important or relevant to your individual organisation, rather than trying to do everything. Some things will be more relevant to certain organisations or sectors than others.
- Have a named HWB lead and/or team with ringfenced time driving the use of the HWB Framework. It can work well to have the team asking stakeholders questions and then completing the diagnostic tool in tandem based on their answers. This may gather less detailed information, but it is enough to identify strengths and gaps.
- Remember that the diagnostic tool is just a tool rather than an end in itself. Aim to create an HWB strategy and supporting practical action plan to guide your investment and changes, and review progress regularly so this is a living process that is part of business as usual.
5.3 Adapt the toolkit to your local needs
- If desired, adapt the tools to fit your local context. For example, to be shorter and more visual to engage a wider range of people or for use in meetings. Organisations can add questions or topics that are priorities locally and simplify some of the wording in diagnostic tool questions if circulating to wider stakeholders.
- Present the results from the diagnostic tool in a simple way, such as short visual reports and graphs.
5.4 Share, collaborate, and support each other as a HWB community
- Share good practice with other local organisations’ HWB leads and help each other overcome challenges. For example, this could be done through two HWB leads buddying up and calling each other once a month, or by several Leads from different organisations meeting – or adopting a community of practice methodology, as within this trailblazer approach.

