2024 Electronic Patient Record (EPR) Usability Survey for secondary care – key findings
The government’s 10 Year Health Plan for England embeds the principle that services will be digital by default – recognising patient choice and addressing usability for staff, maximising outcomes from existing investments, including electronic patient records (EPRs) and advancing digital maturity across the system.
For an NHS fit for the future, we must accelerate bold transformation for the NHS – making digital services the default, recognising patient choice, and addressing usability for staff as a catalyst for sustainable, system‑wide change. A digital-first approach will mean better care, better health outcomes, better patient experience and lower costs.
This is a once-in-a-generation opportunity to make a seismic shift from analogue to digital, transforming care, improving patient and staff experience and becoming a more productive and efficient NHS.
In making a transformational shift, it’s crucial every part of the NHS system understands where they are, where their system partners are and where their peers are in the journey and what are areas for improvement. That’s why we carry out regular assessments of how technology is being adopted across the NHS.
In September 2024, we launched the second national EPR Usability Survey for all secondary care providers. The survey results provided trusts with actionable insights to improve the usability of EPRs for their staff and gave NHS England a detailed understanding of EPR usability to better advocate for future investment in this area.
Key statistics
Total respondents by profession
- Clinicians: 4,524
- Nurses: 6,651
- Allied health professionals: 6,071
- Ambulance staff: 538
- ‘Other’ (including non-clinical): 5,878
Respondents by care setting
- Emergency department: 918
- Inpatient: 5,125
- Inpatient and outpatient: 4,532
- Outpatient: 3,761
- Primary Care: 403
- Ambulance: 1,110
- Community: 5,245
- Mental Health: 2,570
Demographics
The 2024 survey showed a small increase in EPR satisfaction levels overall across English secondary care providers compared with the 3.4* reported in the equivalent survey undertaken in 2021.
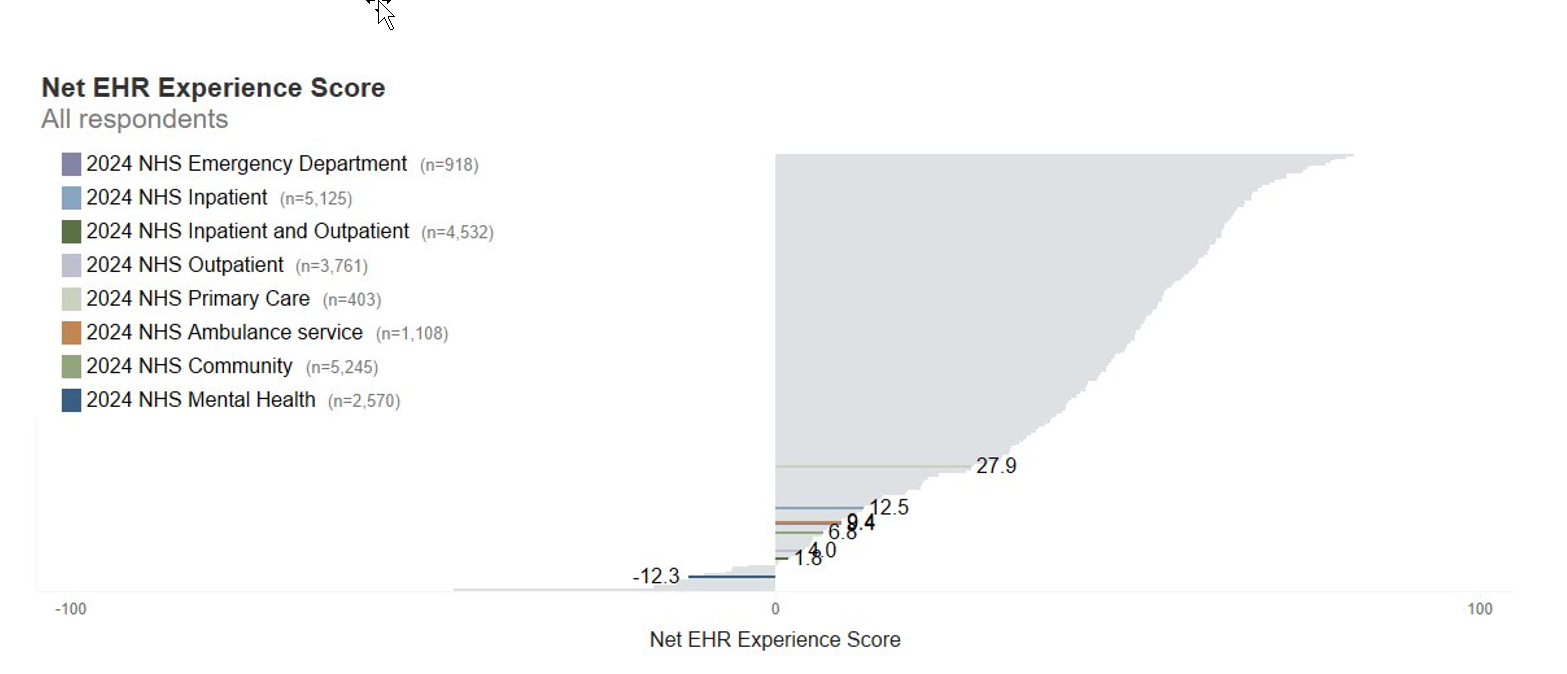
Net EPR/EHR Experience Score by primary setting, all respondents (scale: +100/-100):
- Emergency department – 1.8 (918 respondents)
- Inpatient – 12.5 (5,125 respondents)
- Inpatient and Outpatient – 9.4 (4,532 respondents)
- Outpatient – 4.0 (3,761 respondents)
- Primary care – 27.9 (3,761 respondents)
- Ambulance service – 9.4 (1,108 respondents)
- Community – 6.8 (5,245 respondents)
- Mental health – -12.3 (2,570 respondents)
*Scores are ranked from +100 to -100 and represented as comparative levels with other survey outcomes within the Arch Collaborative data set.
An increase in satisfaction reported by clinicians is offset by a decrease across nursing, health care assistant and allied health professional respondents. These latter groups represent largest cohort of respondents, hence EPR satisfaction has reduced slightly in real terms.
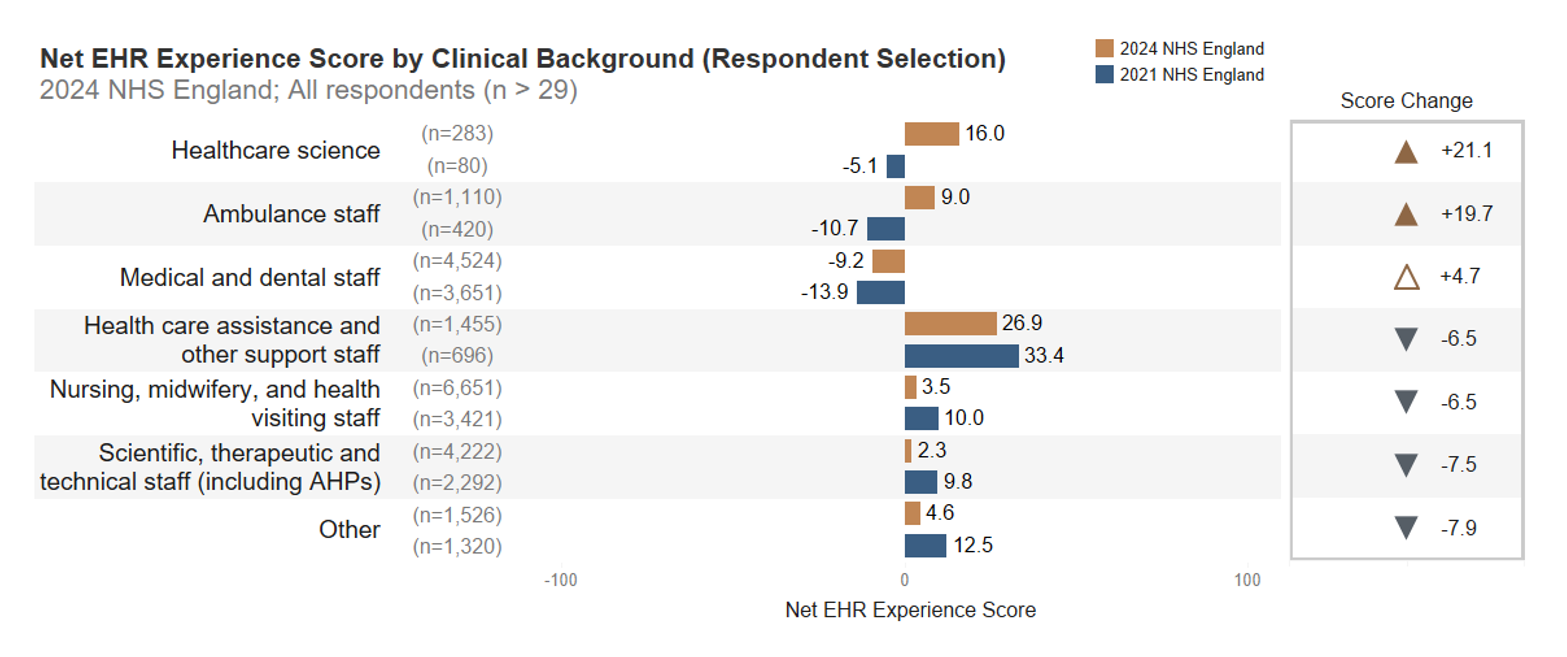
Net EPR/EHR Experience Score by selected clinical background, all respondents (scale: +100/-100)
Healthcare science:
- 2024: 16.0 (283 respondents)
- 2021: -5.1 (80 respondents)
Ambulance staff:
- 2024: 9.0 (1,110 respondents)
- 2021: –10.7 (420 respondents)
Medical and dental staff:
- 2024: –9.2 (4,524 respondents)
- 2021: –13.9 (3,651 respondents)
Health care assistance and other support staff:
- 2024: 26.9 (1,455 respondents)
- 2021: 33.4 (696 respondents)
Nursing, midwifery, and health visiting staff:
- 2024: 3.5 (6,651 respondents)
- 2021: 10.0 (3,421 respondents)
Scientific, therapeutic and technical staff (including AHPs):
- 2024: 2.3 (4,222 respondents)
- 2021: 9.8 (2,292 respondents)
Other
- 2024: 4.6 (1,526 respondents)
- 2021: 12.5 (1,320 respondents)
Conversely, when considering whether clinical practice is enhanced through use of an EPR. Nursing staff are more positive than clinicians with significantly more clinicians strongly disagreeing. Overall, agreement that EPRs support clinical practice is positive.
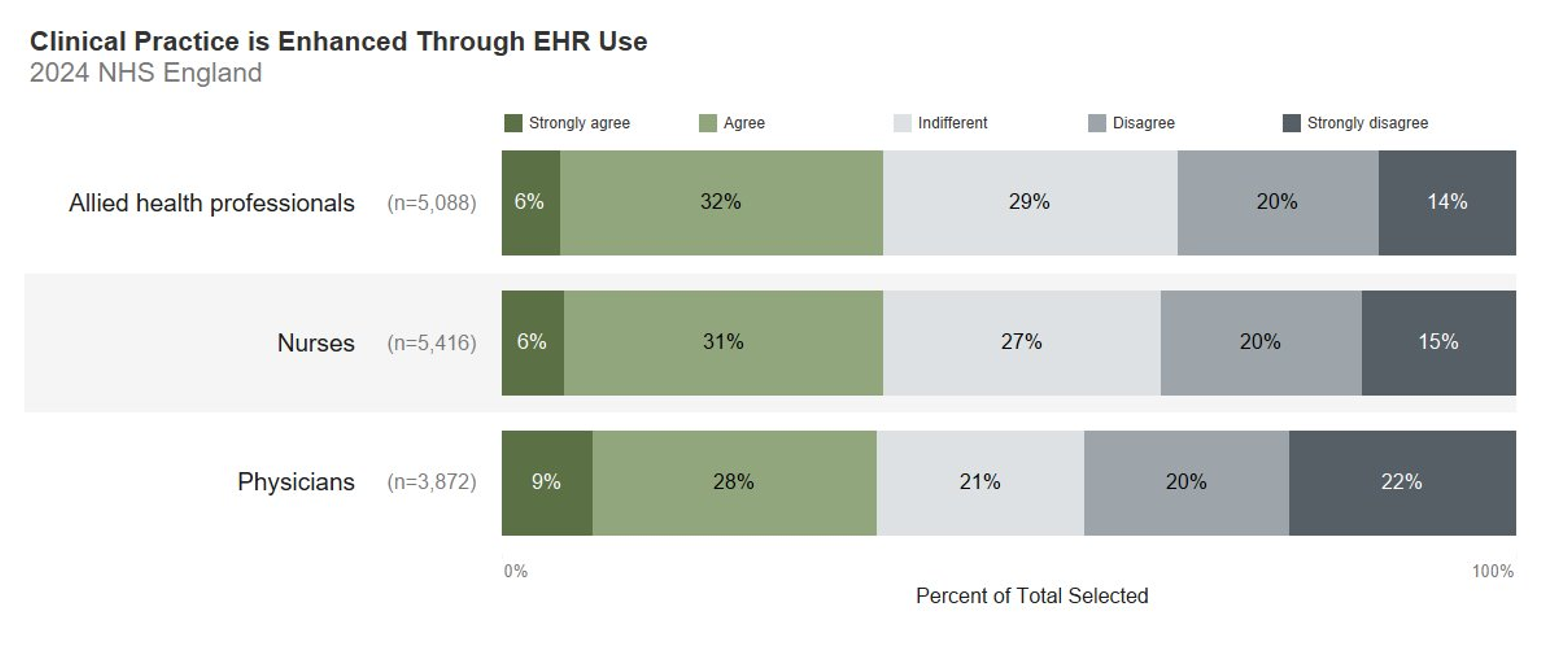
Clinical groups declaration in response to the statement “Clinical Practice is Enhanced Through EHR Use” (scale: percentage)
Allied Health Professionals (5,088 respondents):
- Strongly agree: 6%
- Agree: 32%
- Indifferent: 29%
- Disagree: 20%
- Strongly disagree: 14%
Nurses (5,416 respondents):
- Strongly agree: 6%
- Agree: 31%
- Indifferent: 27%
- Disagree: 20%
- Strongly disagree: 15%
Clinicians (3,872 respondents):
- Strongly agree: 9%
- Agree: 28%
- Indifferent: 21%
- Disagree: 20%
- Strongly disagree: 22%
Key themes for improvement
A key enabler in the shift from analogue to digital is digital leadership and confidence of the workforce. EPR expertise is often recognised a limiting factor in a healthcare providers’ ability to get the best out of both their digital tools and the staff that use them. We need to equip staff with the right skills, whilst providing support to adopt new ways of working.
EPR mastery
EPR mastery refers to the degree to which users can make best use of the capabilities offered by the EPR. Participation in training has shown to increase satisfaction and lead to more efficient use of the EPR [1].
- The survey found that mastery remains low and there is a strong desire from EPR users for more training. 60% of clinicians and 70% of nurses said they wanted more EPR training
- The survey findings suggest that close to half of EPR users do not have formal support or training to help them improve their productive use of the EPR after initial introduction of the system to the organisation – 44% of clinical staff reported receiving no ongoing EPR training at all.
- The task of learning-on-the-job is made more difficult by perceived unintuitive user interfaces presented by the some EPRs – only 38% of clinicians and 42% of nurses consider that their EPR is easy to learn how to use.
Non-optimised workflows
The survey found that the impact of limited EPR mastery amongst frontline users is compounded by digital implementations that, in many instances, are not well-matched with the pathways they support. This leads to a frustrating and inefficient experience that impacts on a care professional’s time that may be more effectively used elsewhere [2].
- Only 34% of survey respondents said that their EPR made them more efficient.
- 48% of clinicians and 43% of nurses report spending three or more hours per week on ‘unproductive charting’. In aggregate, 37% of respondents overall reported sending three or more hours per week on unproductive charting.
- In total 5.2% of all respondents’ working time was reported as lost to unproductive charting (patient record administration that is ‘duplicative or adds no value’).
EPR service delivery
Service delivery of EPRs concerns the provision of the system by the provider organisation, commonly an NHS Trust, and is another aspect of satisfaction that demonstrated an opportunity for improvement. Most suppliers have NHS providers on their installed bases that scored well in overall EPR user satisfaction and others that returned significantly lower scores. It is evident that improvement in satisfaction is possible with the majority of EPR products and that by supporting the providers to develop world-class governance and change management capability, the NHS can realise more of the benefits promised by those EPR systems.
- The mean variance between most positive and most negative overall satisfaction score for each supplier included in the survey was 51 points (percentile range: +100 to -100)
- 61% of respondents reported that they were able to request fixes to their EPR but only 33% agreed the fixes were timely in delivery.
- Respondents were less confident their requests for improvements to the EPR
- 25% of respondents agreed that they felt that they had a voice in the development of their EPR and only 30% agreed that their EPR was
Clinician burnout
In May 2024 The King’s Fund reported that “Vacancies remain a big concern, with an estimated 111,000 posts currently unfilled substantively. Although the NHS workforce has been growing, demand for NHS services has been growing faster, and the health service has not been able to recruit and retain sufficient staff to keep up.”[3]
Analysis conducted by KLAS Research strongly suggests that poor EPR satisfaction is linked to the increased likelihood that clinical staff will leave their role due to feelings of burnout.
The proportion of in England reporting a feeling of burnout is similar to the global average of 33%, but in England they report being more likely to leave their role as a result. They are significantly more likely to attribute their burnout to the EPR getting in the way of their delivery of care than is reported internationally.
- 6,809 clinical staff reported some feelings of burnout in the 2024 survey, which is comparable to the global average of 33%.
- The survey showed turnover rates are higher in England than elsewhere in the world with 8.6% reporting that they intended to leave their role due to feelings of burnout.
Of those clinical staff that reported feelings of burnout:
- 26% plan to leave their current NHS trust in the next two years and while the majority of these stated an intention to continue in healthcare, 18% reported plans to leave healthcare entirely.
- 47% reported that the EPR reduces efficiency while 43% reported that the EPR gets in the way of quality [of care]. These two measures featured within the top 5 user-selected contributors to burnout across all respondents.
Guidance for digital leaders and EPR suppliers
There is a clear positive correlation, in the 2024 survey results and the EPR usability analysis more generally, between the quality of the digital tools provided to clinical and administrative staff and both their efficiency and desire to remain in-post.
Healthcare providers and EPR suppliers are encouraged to use the findings of this EPR user satisfaction survey to inform proactive improvement to the products and services they provide. Healthcare providers can use the information to develop action plans aligned with the key findings and themes to drive improvements that are valuable to their organisations to support all staff using the products.
What survey findings information is available?
Following the closure of the survey, national findings reports were provided to all secondary care healthcare providers in England as follows:
- national findings report – summarising response findings.
- detailed charts – with information from which the summary report was derived.
- raw response data – all the data submitted by each respondent at the provider trust.
- provider dashboard – summarising findings specific to provider organisations that gathered more than 30 responses.
- Supplier report – one or more reports filtered by the supplier(s) for which the organisation holds an active contract.
Useful resources
International research
NHS England’s partnership with KLAS Research includes access for all NHS staff to a significant body of reports, case studies and analysis on topics related to EPR usability, developed using the ARCH Collaborative dataset. KLAS is a globally recognised leader in this field, and this resource offers valuable insight into how healthcare providers worldwide have addressed factors affecting EPR satisfaction and the outcomes achieved.
Guidance on access to the KLAS Research library is available on our Futures collaboration platform.
Case study webinars
Written case studies
NHS England’s Blueprinting programme has developed a comprehensive repository of best practice guidance, including case studies on EPR training, EPR service management, and other related topics. To access the Blueprint library, please register on the Blueprinting Futures collaboration platform
About the survey
The KLAS ARCH Collaborative is a group of healthcare organisations and vendors committed to improving the EPR (also known as electronic health records, or EHRs) experience for clinical staff. The dataset developed through the ARCH Collaborative comprises responses from more than 500,000 user satisfaction surveys across over 300 healthcare organisations worldwide and more than 20 EPR solution vendors. This enables benchmarking against healthcare systems globally (data collection: October 2021–ongoing).
References
- KLAS Research (2023) Clinician Training 2023 – Best Practices for Effective EHR Education.
- KLAS Research (2025) Key Drivers of EHR Improvement 2025.
- The King’s Fund (n.d.) NHS workforce in a nutshell.
