Audit
The benefits of an audit
- Demonstrates good practice for patients and public
- Ensures high standards are met and implements changes when needed
- Ensures compliance with Health and Social Care Act (205)
- Ensures compliance with antimicrobial stewardship
Updated Audit tools
Individual audit of antimicrobial prescribing activity Use this audit tool to measure your own antimicrobial prescribing practice against recommended guidelines.
Wider audit of dental infection management Use this audit tool to assess the management of dental infection in practice. This can be used for multiple clinicians or across a practice.
Coming soon – Secondary care audit tools
The Audit Process
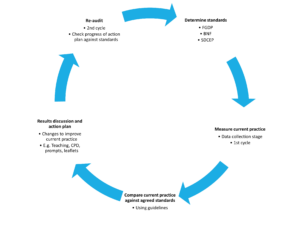
How to use the audit tools
- Read up on the guidelines (FGDP/BNF/SDCEP)
- Set an agreed standard (i.e. 90% of prescriptions must met guideline criteria)
- Decide whether your audit will be prospective (current practice) or retrospective (past practice).
- 1st cycle: complete data collection using excel spreadsheet over the course of 1-2 months.
- Compare data against agreed standards and record whether standard is met or not.
- Results discussion with team and action plan. Changes should be implemented to improve current practice (using SMART guidance) over at least 1-2 months.
- 2nd cycle: RE-AUDIT. Complete data collection using excel spreadsheet over the course of 1-2 months. Compare data against agreed standards.
- If standards are met – audit cycle can be closed but revisited to ensure continuing compliance.
- If standards are not met – 3rd audit cycle to be undertaken as discussed until standard is met.
Original audits designed in collaboration between PHE, FGDP, and BDA. Updated for your use (Dental subgroup of ESPAUR, 2016) (Public Health England, 2016).
