Maternity Transformation Programme
Better Births, the report of the National Maternity Review was published in February 2016 and set out a clear vision: for maternity services across England to become safer, more personalised, kinder, professional and more family friendly; where every woman has access to information to enable her to make decisions about her care; and where she and her baby can access support that is centred on their individual needs and circumstances. It also calls for all staff to be supported to deliver care which is women centred, working in high performing teams, in organisations which are well led and in cultures which promote innovation, continuous learning, and break down organisational and professional boundaries.
Implementing the vision set out Better Births will support the Secretary of State’s ambition to halve the number of stillbirths, neonatal and maternal deaths and brain injuries by 2030.
Since the publication of Better Births in 2016 and of the Report of the Morecambe Bay Investigation in 2015, the NHS and its partners have come together through the national Maternity Transformation Programme to implement its vision for safer and more personalised care across England and deliver the national ambition to halve the rates of stillbirths, neonatal mortality, maternal mortality and brain injury by 2025. As we reach the fourth anniversary, this is an opportune time to take stock of progress, to reflect on successes and remaining challenges, and consider where further action is needed.
Better Births Four Years On: A review of progress
The Maternity Transformation Programme
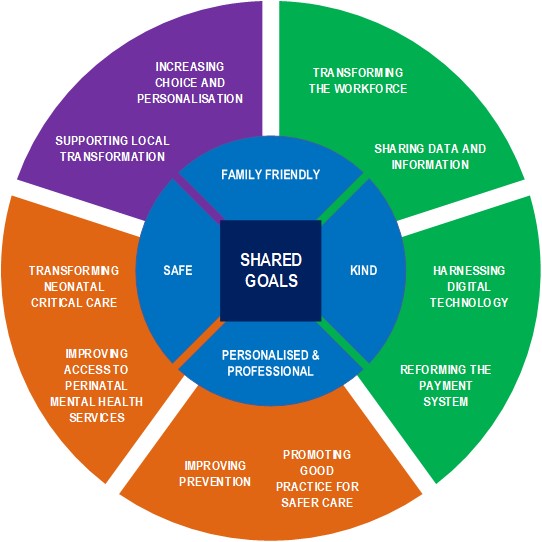
The Maternity Transformation Programme seeks to achieve the vision set out in Better Births by bringing together a wide range of organisations to lead and deliver across 10 work streams. The programme is led by a Programme Board, supported by a representative group of stakeholders that will scrutinise and challenge decisions made by the Board.
Local transformation supported by national enabling action is key to realising the Better Births vision. Providers and commissioners of maternity services have formed Local Maternity Systems, which will plan the design and delivery of services of populations of 500,000 – 1,500,000 people.
Ten national programme work streams are supporting the implementation of Better Births locally:
Local drivers for change
Supporting local transformation: working in tandem with ICSs, and through the maternity Clinical Networks and regional boards, to provide targeted support to local maternity systems. Support for seven Early Adopters has harnessed enthusiasm for change and tested the model of care described in Better Births. Over 100 Maternity Voices Partnerships have now been established across England. There are over 100 community hubs in operation, providing a range of services wrapped around the woman and her family, and we have a renewed focus on postnatal care. So far we have expanded access to continuity of carer pathways for pregnant women so that 17.3% of pregnant women were placed onto a continuity pathway in March 2019. We are working to increase continuity of carer for certain BAME groups and women living in the most deprived areas.
Increasing choice and personalisation: we have concluded working with seven Maternity Choice and Personalisation Pioneers to test new approaches to widen and deepen choices available to women through personal maternity care budgets. Evaluation for this is now available. All women can expect to be offered a personalised care and support plan by 2021.
Service improvement
Promoting good practice for safer care: there is much good practice already in the NHS and this work stream aims to ensure widespread dissemination and adoption of best practice, through targeted support to embed a safety, learning and improvement culture throughout NHS maternity services. This includes a commitment to achieve the ‘halve it’ ambition for maternal deaths, neonatal deaths, still birth and brain injury. The Saving Babies’ Lives Care Bundle evaluation showed a 20% decrease in stillbirths in the early implementer sites, and a SBLCBv2 has been launched to include action on avoiding preterm birth. We are also working to address the variation in outcomes for certain BAME groups and women living in the most deprived areas. This year we have achieved our target of reducing the number of stillbirths by 20% 3 years early and put actions in place to help us deliver our target of reducing maternal mortality, neonatal mortality and serious brain injuries.
Improving access to perinatal mental health services: this is a joint work stream between the Maternity Transformation Programme and the Mental Health Programme. It aims to improve access for women to high-quality specialist mental health care, closer to home, when they need it during the perinatal period. Four new Mother and Baby Units have been established and every ICB now has access to specialised community perinatal mental health services. We now need to deliver the commitments of the NHS Long Term Plan for outreach clinics to address moderate to severe or complex perinatal mental health needs across the country, which will be taken forward initially in the form of pilots.
Improving prevention: led by Public Health England, work is aimed at preventing poor outcomes through actions to improve women’s health – before, during and after pregnancy to ensure that families get off to the best start possible. PHE published the report ‘Making the case for preconception care’ in July 2018. The report covers the impact of preconception health and ways to improve outcomes and reduce inequalities. In addition to this ALBs have worked together to give all trusts the opportunity to benefit from training to reduce maternal smoking.
Transforming neonatal critical care: This is a joint venture between Specialised Commissioning and the Maternity Transformation programme. It aims to improve neonatal outcomes by aligning capacity and demand, developing the neonatal workforce and improving parental support. With the publication of the Neonatal Critical Care Review (NCCR) Action Plan all systems should update their final implementation plans for addressing local neonatal critical care capacity. Targeted funding will be available from 2020/21 to support the expansion and improvement of some of these services through the NHS Long Term Plan.
System enablers
Transforming the workforce: led by HEE this workstream aims to ensure we have the right workforce with the right skills to implement the vision set out in Better Births. This has included multi-professional training packages, a competency framework for Maternity Support Workers, and expanding midwifery training placements by 25% over four years.
Sharing data and information: we are working with partners to improve data and information collection, quality and sharing to drive maternity service improvement at local, regional and national levels.
Harnessing digital technology: led by NHS X, this work stream is facilitating the development and rollout of patient-held digital maternity records to support women to manage their care. As of September 2019, 105,000 have been offered access their digital maternity record, with 60% of these women accessing the record. This is ahead of the original target date of April 2020.
Reforming the payment system: having made some tweaks to the existing tariff to support implementation of Better Births, NHS England is now developing more radical reform based on a blended payment model. Once confirmed, the focus will be on supporting Local Maternity Systems to make the most of the opportunity.
Stay connected
Delivering the Better Births vision is reliant upon a wide range of organisations and stakeholders working together and embracing change to ensure high-quality services for women, babies and their families.
As well as being involved in shaping services locally, here are some of the ways you can keep in touch with the latest news and developments:
-
-
- Follow us on twitter – @NHSEngland and use our dedicated hashtags to follow and contribute to the conversation #BetterBirths #MatExp #SavingBabies.
- Keep an eye on our web pages for the latest news and events
- Watch out for Maternity Transformation blogs and bulletin issues.
-
For general questions and queries, please drop us a line, england.maternitytransformation@nhs.net.