Resources
Resources to support implementation of modern general practice
- Assessment tool for modern general practice
- How to improve care navigation in general practice
- How to align capacity with demand in general practice
- How to improve telephone journeys in general practice
- How to improve care related processes in general practice
- Modern general practice webinars
- Administrative triage using digital tools in general practice
- National care navigation training for general practice staff
- Demand and capacity webinar sessions for general practices and primary care networks
- Getting started series guides
Patient online journeys through GP websites and online consultation tools
- Step-by-step guide to improving general practice website online journeys
- Creating highly usable and accessible GP websites for patients
- GP website benchmarking and improvement tool
- 10 top tips for supporting digital inclusion in general practice
Clinical resources to support remote and online consultations
- How to conduct written online consultations with patients in primary care
- Principles of safe video consulting in general practice during Covid-19
- Key principles for intimate clinical assessments undertaken remotely in response to COVID-19
- Using online consultations in primary care – implementation toolkit
Online networks to support general practice transformation and improvement
Quality improvement resources
Resources to support communication with patients
Step-by-step guide to improving general practice website online journeys
A guide for those responsible for planning, leading and maintaining GP website improvement work within practices, primary care networks (PCNs), GP federations, integrated care boards (ICBs) and other organisations.
This guidance will help you with:
- understanding the elements of an improvement plan and the information you need to collect
- benchmarking the usability of current online patient journeys
- making a plan for improvement
- delivering and maintaining that improvement.
Read or download this guide: NHS England » Step-by-step guide to improving general practice website online journeys
Assessment tool for modern general practice
Review and improve your general practice processes with the Assessment Tool for Modern General Practice. It helps practices reflect on their current processes—highlighting what’s working well and where improvements can be made. It’s flexible, non-prescriptive, and has built-in links in each section to step-by-step improvement support.
Read or download this tool: NHS England » Assessment tool for modern general practice
How to review and improve your assess, prioritise and allocate processes in general practice: care navigation
This comprehensive guide supports general practices to review and enhance their assess, prioritise and allocate processes (sometimes referred to as care navigation). Whether facing rising patient demand, staff burnout, or challenges with access and continuity of care, this guide offers a practical, step-by-step approach to assess, prioritise and allocate patients to help them reach the right care, first time. You can follow the guidance end to end if you want to develop an entirely new care navigation process. If you already have a process in place and want to improve or add certain elements, you can simply dip into the relevant sections.
The guide includes access to editable resources to save practice staff time.*
Read or download this guide: NHS England » How to improve care navigation in general practice
How to align capacity with demand in general practice
This guide is for general practice teams who are seeking to better understand, manage and align demand and capacity in their practice.
Building data collection and data analysis capabilities provides practices with the skills to be able to understand demand and capacity, which in turn supports practices to tackle many different, but often inter-connected challenges for example:
- peak demand on the phone
- running out of appointments during the day
- overwhelming demand on GP appointments
- a rising ‘queue’ of non-urgent appointments
Read or download this guide: NHS England » How to align capacity with demand in general practice
Creating highly usable and accessible GP websites for patients
This guidance is for practice managers, primary care networks (PCNs), integrated care systems (ICSs), GP federations and anyone who is looking for guidance for improving general practice (GP) websites.
There are multiple benefits to creating a highly accessible and usable GP website. It will:
- improve patient satisfaction and experience of using the GP practice, making it more likely they will return and use digital tools
- ensure patients are signposted to the correct place for their needs, reducing wasted patient and practice time
- reduce the risk of adding digital inequalities to existing health inequalities
- remove access barriers for patients with disabilities and make your website legally compliant
- create a place where patients can effectively self-serve, thereby:
- reducing the burden on receptionists and clinical staff
- empowering patients to manage their health and care
- creating highly usable and accessible GP websites for patients
Read our research in full on the FutureNHS platform (requires a login)
GP website benchmarking and improvement tool
The GP website benchmarking and improvement tool has been developed to support integrated care systems (ICSs), primary care networks (PCNs) and general practice teams to audit the usability of key patient web journeys. The tool provides a deeper understanding as to whether a GP website meets a high standard of usability along with contractual requirements laid out in the GS contracts and other requirements of practices.
You can use the tool to:
- create a checklist of improvements needed.
- identify which elements for improvement are usually the responsibility of the website supplier or the practice.
- audit a site before and after usability changes are made to measure improvements.
- compare the usability of two or more sites.
How to improve telephone journeys in general practice
High quality, effective telephone and online journeys are key enablers of modern general practice. They should integrate well with and support care navigation and administrative processes within a practice or primary care network (PCN).
This guidance helps practices and PCNs choose, purchase and optimise the use of advanced cloud-based telephony.
Read or download this guide: NHS England » How to improve telephone journeys in general practice
How to improve care related processes in general practice
Well designed and integrated care related processes can bring significant time savings for practices and improve patient experiences.
This guidance offers information on three important care-related activities (workload that pertains to a patient but does not directly involve them):
- prescription management
- long-term condition recalls
- new patient registration
In addition, it also offers improvement approaches which can be applied to a wider range of tasks and processes in general practice.
Read or download this guide: NHS England » How to improve care related processes in general practice
Modern general practice webinars
A series of webinars to support the implementation of modern general practice is available on Connect – our online space on Future NHS (login required).
Remote versus face-to-face: which to use and when?
Tip and learning to support clinicians when choosing a consultation modality.
Access or download this guide, published by the Royal College of General Practitioners.
How to conduct written online consultations with patients in primary care
A visual summary of tips for effective online consultations published by BMJ.
Read or download this information, published by BMJ.
Principles of safe video consulting in general practice during COVID-19
This guidance for NHS general practice staff who are consulting via video with patients at home. Practitioners are expected to have full access to the patient’s primary care medical record and to be consulting with patients in England.
Read or download this guide: Coronavirus » Principles for supporting high quality consultations by video in general practice during COVID-19.
Key principles for intimate clinical assessments undertaken remotely in response to COVID-19
The principles in this guidance aim to support patients to access care in a way that meets their needs and to support clinicians to provide care in a way that is in the best interests of their patients, whilst protecting both from the risks associated with remote intimate assessments.
Administrative triage using digital tools in general practice
The administrative triage using digital tools in general practice eLearning module has been designed to support general practice administrative staff to design their practice workflow in sorting, signposting and delivering administrative triage with the aim of supporting an inclusive approach to managing demand and workload.
Consisting of nine modules, it has been developed in collaboration with the Practice Managers Association.
Using online consultations in primary care – implementation toolkit
The online consultations implementation toolkit has been developed to support practices, clinicians, commissioners and PCNs with the successful adoption of online consultation systems and the seamless integration of these alongside face-to-face and other services.
There is both a full version of the toolkit for those who are leading these projects and a shortened version, particularly aimed at GPs and other practice staff. The toolkit is an interactive and provides a range of ideas and options for different professionals, including clinicians, at different points in their implementation journey. As a result, those using the toolkit are encouraged to jump through to the sections most relevant to their role or organisation.
10 top tips for supporting digital inclusion in general practice
This guide, Supporting digital inclusion in general practice: 10 top tips, is for healthcare staff in general practices, primary care networks (PCNs), integrated care systems (ICSs) and anyone who is seeking to improve digital inclusion in general practice, particularly among under-served and marginalised communities. It has been produced in partnership with the Good Things Foundation, a digital inclusion charity and draws on examples of good practice in 30 primary care and community-based organisations.
Inclusive access routes to general practice – support for surgery teams
This tested toolkit of materials (fully updated in April 2023) is to help practice teams explain to patients the 3 ways they can get in touch to get the care they need – by phone, in person or using an online form on the practice’s website (sometimes referred to as online consultation requests). It aims to build patient understanding of using digital routes and confidence in using them and in how their practice will respond.
General Practice Access Routes is free to download (login required). It includes:
- posters, counter cards, leaflets for reception areas
- useful tips, help and links from practices.
Primary care improvement community
The primary care improvement community is a community for all who work in and around general practice and primary care across England, and are involved in facilitating innovation, improvement and transformation. This spreads good ideas more quickly, helping to accelerate local change and support change leaders in sustaining progress and their own resilience.
To join the community, please sign up to: Connect – our online space on FutureNHS (login required).
Digital primary care community
The Digital Primary Care FutureNHS site (requires login) provides a platform for NHS colleagues working within digital primary care to come together and share experiences, learning and resources. Joining the network gives you access to an online hub of resources, guidance and case studies to support digital transformation of primary care services. With more than 6,000 members it also provides a great opportunity to share issues, questions and solutions with colleagues through online discussions.
National care navigation training for general practice staff
The Delivery plan for recovering access to primary care, committed to training 6,500 general practice staff (one person from every practice in the country) in care navigation skills. Practice and PCN managers can nominate one member of staff, ideally reception staff and care navigators involved in managing patient requests, to complete the virtual care navigation training. It’s anticipated that this will be a popular programme and that spaces will fill up quickly.
On completion, individuals will be confident to communicate effectively with patients and be able to signpost to the most relevant team member or local services depending on patient needs. An advanced training offer will be available at a later date for those with experience of care navigation who can support and embed it into practices and networks for sustainability and standardisation. If you have any questions or would like more information, visit the Care navigation training online space on FutureNHS (login required).
Demand and capacity webinar sessions for general practices and primary care networks
This series of webinars on Future NHS (login required) is a resource to support practices and PCNs to develop skills and confidence with using quality improvement tools and techniques, focused on demand and capacity.
Change Model
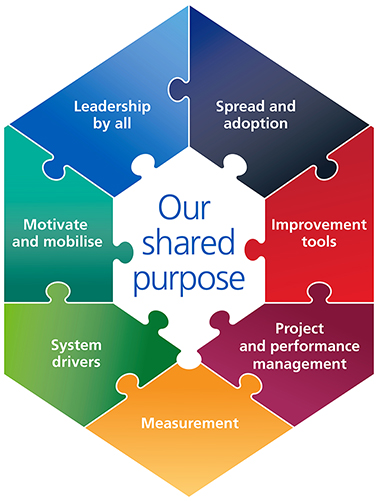
The Change Model is a framework for any project or programme that is seeking to achieve transformational, sustainable change.
The model, provides a useful organising framework for sustainable change and transformation that delivers real benefits for patients and the public. It was created to support health and care teams and organisations to adopt a shared approach to leading change and transformation.
The model has eight components, all of which should be considered when implementing change. The components act as a guide to ensure all elements of change are considered and implemented effectively, creating an environment where change programmes deliver transformational, sustainable change.
The Change Model was developed with hundreds of senior leaders, clinicians, commissioners, providers and improvement activists who want to get involved in building energy for change across health and care by adopting a systematic and sustainable approach to improving quality of care.
We have recently refreshed and enhanced the model to include a PDF guide and a series of supporting diagnostic tools to use in your work, including an action planning template and a key questions template for each component of the guide:
- Change Model guide
- Change Model action planning template
- Change Model GAP analysis tool
- Our shared purpose – key questions
- Spread and adoption – key questions
- Improvement tools – key questions
- Project and performance management – key questions
- Measurement – key questions
- System drivers – key questions
- Motivate and mobilise – key questions
Getting started series guides
The ‘Getting Started’ series is designed to help you think through how you are going to approach any improvement you want to make in practice. You can access these resources on Connect – our online space on Future NHS (login required).